People often expect grief to look like crying at a funeral. Real life is usually messier than that. You might feel numb after a breakup, angry after a family move, distracted after losing a pet, or unexpectedly calm right after hearing bad news. Then, hours later, it hits you while you are brushing your teeth or trying to finish an assignment online. Grief does not only happen after death, and it does not always look dramatic. It can show up quietly, physically, and unexpectedly.
Learning how to handle grief matters because loss and major change are part of life. If you do not have strategies for these moments, stress can spill into sleep, relationships, schoolwork, motivation, and safety. But when you learn practical ways to cope, support others, and ask for help, you build something important: the ability to stay steady during hard times without pretending you are fine.
Grief is your response to losing someone, something, or a version of life you cared about. That could mean a death, but it can also mean your parents separating, moving away from your community, losing a friendship, going through a serious illness, ending a relationship, or having a major plan fall apart. A big transition can bring grief even if the change is not completely negative. For example, moving to a better home can still mean losing familiar places and routines.
When life changes fast, your brain and body may go into stress mode. That can affect sleep, appetite, focus, energy, and patience. You may feel like you should be able to "just deal with it," especially if other people seem to be moving on. But emotional recovery is not a competition. Your experience is real even if someone else has it worse.
Grief is the emotional, mental, physical, and social response to loss. Resilience is the ability to adapt, recover, and keep functioning during or after difficult experiences. Transition means a major change in life circumstances, roles, or routines.
One of the most helpful things you can remember is that strong feelings are not proof that you are weak. They are signals that something important has changed. Your job is not to erase those signals instantly. Your job is to notice them, respond safely, and keep taking care of yourself.
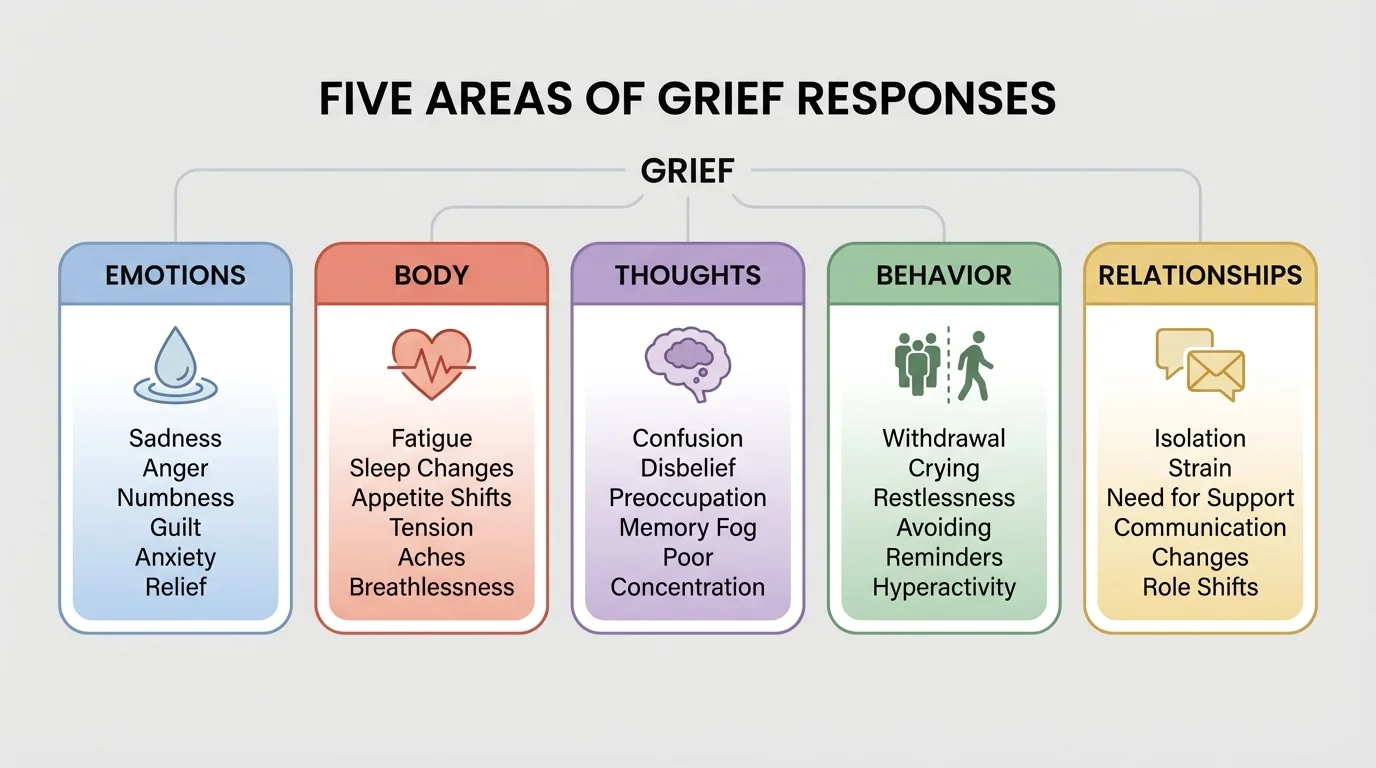
Grief can affect much more than feelings, as [Figure 1] shows. You might notice changes in your emotions, body, thoughts, actions, and relationships all at once. That is one reason grief can feel confusing: you may think something is wrong with you when you are actually experiencing a normal response to loss.
Emotionally, you might feel sadness, anger, guilt, relief, fear, loneliness, or numbness. Physically, grief can show up as headaches, stomachaches, tiredness, trouble sleeping, or feeling restless. In your thinking, you may have a hard time focusing, forget simple things, replay memories, or wonder whether you could have changed what happened. Socially, you may want extra connection or want everyone to leave you alone.
There is no perfect order to grief. Some people cry right away. Some do not cry for weeks. Some people talk a lot. Others go quiet. You might feel okay in the morning and terrible at night. You might laugh at a memory one minute and feel angry the next. None of that automatically means you are grieving the wrong way.
A lot of people have heard of "stages of grief," but real grief is not a neat staircase. It is more like weather: it changes, returns, and sometimes surprises you. That is why it helps to track patterns instead of judging each moment. For example, if you notice that evenings are harder, social media makes things worse, or certain songs bring up strong feelings, you can plan around that instead of being caught off guard.
Grief can also change behavior. You may oversleep, stop replying to messages, scroll for hours, snap at people, or try to stay busy every second so you do not have to feel anything. Some coping behaviors give short-term relief but create bigger problems later. Ignoring everyone, using substances, self-harming, or posting very personal pain online in unsafe ways can leave you feeling worse and less supported.
Grief sometimes includes relief. If someone was very sick or a situation had been stressful for a long time, feeling relief does not mean you did not care. Mixed emotions are common.
As the pattern in [Figure 1] makes clear, grief is not just "being sad." It can affect sleep, concentration, motivation, and relationships. That is why healthy coping needs to support your whole life, not just your mood.
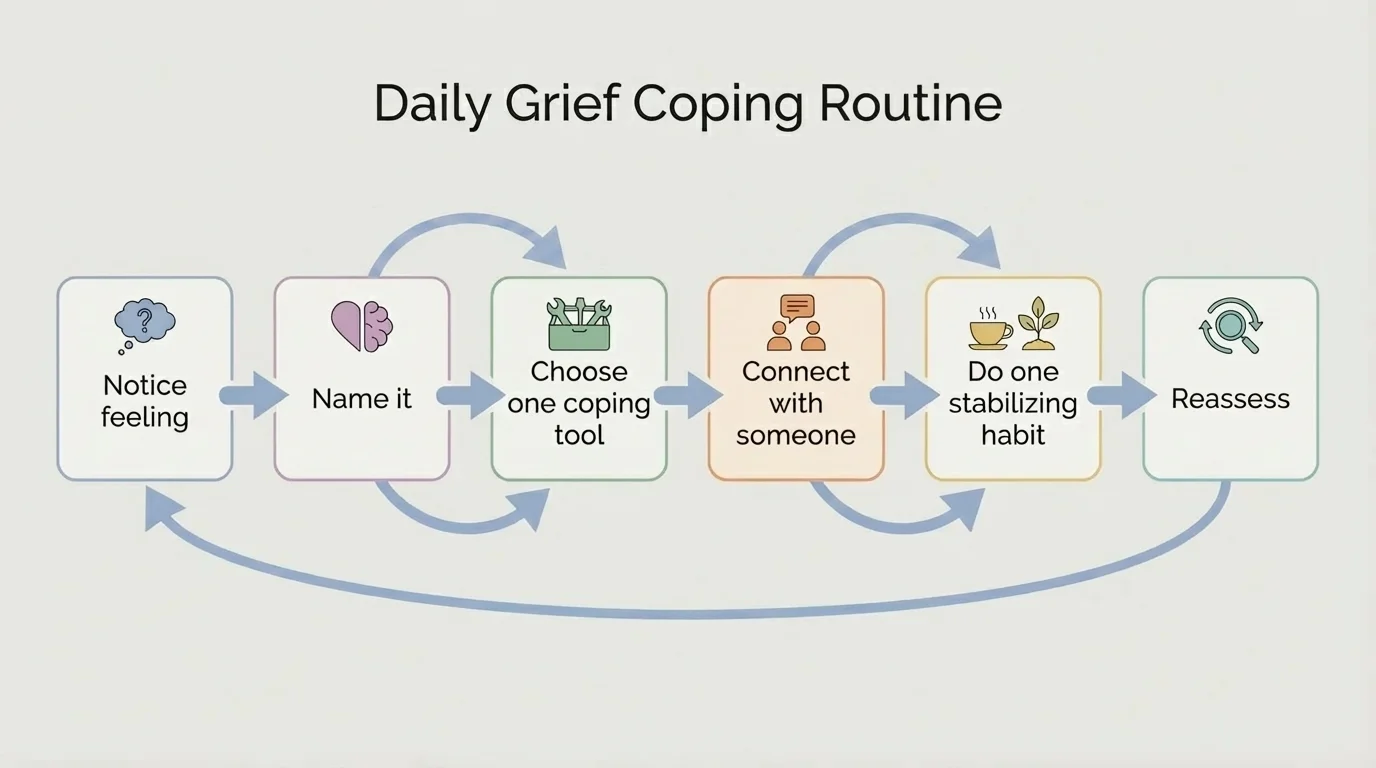
[Figure 2] outlines a practical routine for processing grief. When people hear "process your feelings," it can sound vague. A more useful approach is to notice what is happening, name it, choose one safe coping tool, connect with someone, and do one stabilizing action. You do not need to fix everything at once. You just need your next steady step.
Step 1: Notice what is happening. Pause and ask yourself, "What am I feeling right now?" If you cannot find the exact word, start broad: sad, angry, scared, numb, overwhelmed. Naming a feeling can make it less chaotic.
Step 2: Check your body. Ask, "Have I slept? Eaten? Had water? Been outside? Been online too long?" Sometimes emotional pain gets amplified when basic needs are ignored. Taking care of your body is not avoiding grief. It is giving yourself the strength to handle it.
Step 3: Express instead of bottling up. You do not have to share everything publicly. Expression can be private. You might journal, voice-note your thoughts, make art, pray, talk during a video call, write a letter you never send, or create a playlist that matches your mood. The goal is to let the feeling move, not get stuck.
Step 4: Use grounding when feelings spike. Grounding helps when emotions become so strong that you feel flooded. Try the grounding technique called the 5-4-3-2-1 technique: name five things you see, four you feel, three you hear, two you smell, and one you taste. This brings your attention back to the present moment.
Step 5: Keep a basic routine. Grief often knocks life off schedule. Try to protect a few anchors: wake-up time, meals, school check-ins, hygiene, movement, and sleep. You do not need a perfect day. You need enough structure to keep from drifting.
Step 6: Create a memory ritual if the loss involves someone or something meaningful. You might keep a photo, light a candle with family, save voice messages, plant something, make a digital album, or write down stories you do not want to forget. Rituals can help you stay connected without being stuck.
Practical coping example
You feel overwhelmed at night after your parents tell you a major family change is coming.
Step 1: Name the experience
You say to yourself, "I am not just tired. I am scared and unsettled because things are changing."
Step 2: Lower the intensity
You put your phone down for ten minutes, drink water, and do slow breathing: inhale for a count of four, hold for a count of four, exhale for a count of six.
Step 3: Express safely
You write three sentences in a notes app about what feels uncertain and what support you need.
Step 4: Reach out
You text a trusted adult: "I am having a hard time with this change and could use a check-in tomorrow."
Step 5: Protect tomorrow
You set out what you need for the morning and choose one manageable task for the next day so everything does not feel impossible.
Healthy coping is not the same as pretending to be positive. It is okay if some days you feel productive and other days you do not. What matters is avoiding coping methods that create more harm. If you notice that you are missing meals, isolating completely, lashing out online, using substances, or hurting yourself, that is a sign to involve support quickly.
Boundaries matter too. During grief, some people want to talk a lot, and some do not. You are allowed to say, "I appreciate you checking in, but I do not want to discuss details right now," or "Texting is easier for me than calling today." Healthy support respects your limits.
Later, when you need to repeat the process, [Figure 2] still applies: notice, name, cope, connect, stabilize, reassess. Simple systems help when your mind feels overloaded.
When someone you care about is grieving, you do not need the perfect speech. Most people remember whether you were kind and consistent, not whether your words were flawless. Supporting someone well means showing empathy, respecting their pace, and avoiding the urge to control their emotions.
A good starting point is simple and honest: "I am sorry you are going through this," "I care about you," or "I am here if you want to talk." If you are close to the person, be specific. Instead of saying, "Let me know if you need anything," try, "Do you want me to check in tonight?" or "Would it help if I stayed on a call while you work?" Specific support is easier to accept.
Here are some helpful guidelines:
Helpful support sounds like presence, not pressure. The goal is not to make grief disappear. The goal is to make the person feel less alone, less judged, and safer to be honest. Real support often looks ordinary: listening, remembering important dates, sending a short message, or staying calm when someone is upset.
It is also important to respect differences. Culture, religion, family habits, personality, and the type of loss all affect how people grieve. One person may want to post a tribute online. Another may want privacy. One may talk openly. Another may process through music, prayer, exercise, or time with family. Support should fit the person, not your idea of what grief should look like.
If your friend says something that worries you, take it seriously. If they talk about self-harm, wanting to disappear, not wanting to be alive, or feeling unsafe at home, do not promise secrecy. Tell a trusted adult or crisis service right away. Being a good friend includes getting help when the situation is too big for you to handle alone.
What to say and what to avoid
Suppose a friend messages you that their grandparent died and they do not know what to do.
Better response: "I am really sorry. You do not have to answer right away, but I am here. Want me to check in later today?"
Why it helps: It shows care, gives space, and offers a clear next step.
Less helpful response: "At least they lived a long life" or "You need to stay strong."
Why it hurts: It can make the person feel rushed, dismissed, or unable to be honest.
Not every major transition is a death or obvious tragedy. You may grieve when a parent remarries, when you move, when your health changes, when a friendship ends, when your family finances shift, or when your role in the family changes. You can even grieve after a good change because good changes still involve endings.
This is where resilience becomes practical. Resilience is not "never getting upset." It is the skill of adjusting without losing yourself completely. That means noticing what has changed, accepting what you cannot control, and taking action on what you can control.
A useful approach during transition is to sort your situation into three groups:
This kind of sorting can lower stress because it gives your mind somewhere useful to focus. If you spend all your energy fighting what is already decided, you may feel powerless. If you act on what is still possible, you build momentum.
Emotional regulation does not mean shutting feelings off. It means recognizing them, reducing their intensity when needed, and choosing your next action on purpose instead of reacting automatically.
Transitions also often affect identity. You may wonder, "Who am I if my family looks different now?" or "Who am I if that friendship ended?" Those questions are real. Give yourself time. Major change can temporarily shake your sense of normal, but it can also help you learn what matters to you, what support you need, and what kind of person you want to be.
Try to reduce unnecessary pressure during transition periods. If possible, lower your expectations for perfection and raise your expectations for support. That might mean breaking school tasks into smaller parts, communicating early when you are struggling, and making a short daily plan instead of a huge one.
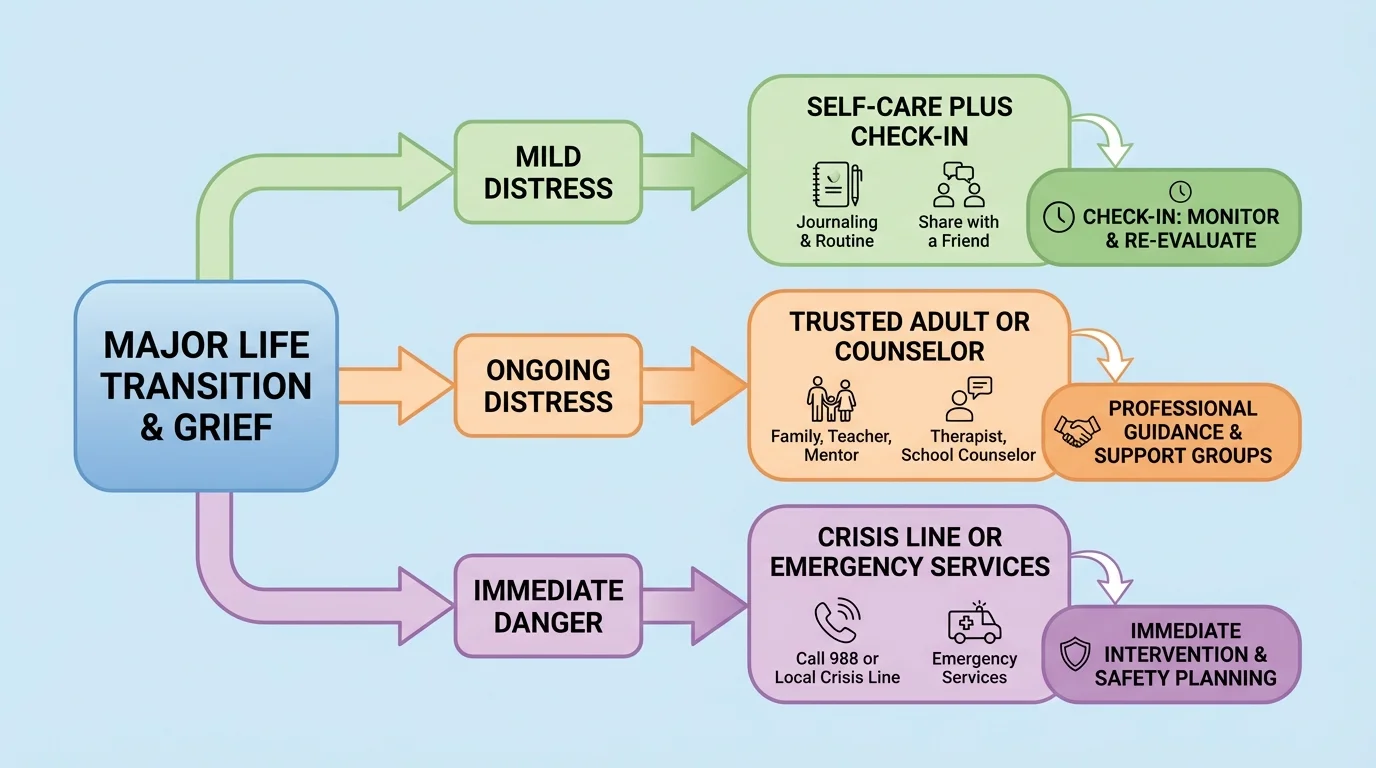
[Figure 3] shows different support paths for mild distress, ongoing distress, and urgent danger. Some grief and stress can be handled with personal coping tools and support from people you trust. Other situations need more help. Asking for help is not overreacting. It is a smart response when your usual coping tools are not enough.
Seek extra support if grief or transition stress is lasting a long time without easing at all, interfering with sleep or eating, making it hard to function most days, causing panic, leading to self-harm, or making you feel hopeless. Also seek help if the loss connects to trauma, abuse, violence, or an unsafe home situation.
Trusted support can include a parent, guardian, relative, coach, youth leader, therapist, doctor, school support staff in your online program, or another dependable adult. If one person does not respond well, try another. Not getting the right response the first time does not mean you should stop reaching out.
Here is a simple script you can use: "I have been having a hard time since this loss/change. It is affecting my sleep, focus, and mood, and I do not think I should handle it alone. Can we talk about support?" You do not need a dramatic speech. Clear and direct is enough.
If speaking feels hard, send a message instead. You could write: "I need help. I have been feeling overwhelmed and I want to talk today." Short messages are fine. The important thing is making contact.
How to ask for help
Step 1: Pick one trusted person
Choose someone who is usually calm, respectful, and likely to take you seriously.
Step 2: Name the issue clearly
Say what is happening: grief after a death, stress after a move, panic after a breakup, or constant sadness after a family change.
Step 3: Give one or two signs
Examples: "I cannot sleep," "I keep crying," "I am shutting down," or "I do not feel safe with my thoughts."
Step 4: Ask for a next step
Examples: "Can you help me find counseling?" or "Can you stay with me while we call someone?"
If you ever think you might hurt yourself, or if you feel like you cannot stay safe, skip the "maybe I should wait" debate. Tell a trusted adult immediately, contact emergency services, or use a crisis hotline or text line in your area right away. Urgent safety concerns need urgent action.
Later, if you need to decide what level of support fits the situation, [Figure 3] gives a useful guide: mild distress may call for coping tools and check-ins, ongoing distress points to a trusted adult or professional, and immediate danger means emergency or crisis support now.
"Asking for help is a strength skill, not a weakness sign."
When emotions are high, it helps to have a plan before the next hard moment happens. Keep it simple enough that you could actually use it on a bad day.
1. My warning signs: List three signs that tell you you are not okay, such as not sleeping, isolating, crying every night, getting angry fast, or having scary thoughts.
2. My calming tools: Choose three safe strategies, such as grounding, journaling, music, a shower, movement, prayer, breathing, or talking to someone.
3. My support people: Write down at least two names and how to contact them.
4. My daily anchors: Pick a few basics you will protect even on rough days: food, water, hygiene, one school task, fresh air, and sleep.
5. My emergency step: Decide now what you will do if you feel unsafe: who you will tell, which hotline you will use, or which adult you will go to immediately.
This plan does not erase grief. It gives you a structure so grief does not run your whole life. You can still feel deeply and act wisely at the same time.
Try This: Save a note in your phone titled Hard Days Plan. Add your warning signs, three coping tools, and two people you can contact. If supporting a friend, save one sentence you can send, such as "I care about you, and I can stay with you while we find help." Small preparation can make a big difference when emotions are intense.