Most people do not make their worst decisions because they are careless. They make them because stress, panic, hopelessness, or exhaustion narrows their thinking. That is exactly why a mental health crisis plan matters. You do not create it during your hardest moment. You create it now, while you can think clearly, so future-you has instructions, support, and a safer path forward.
A personal mental health crisis plan is not only for someone with a diagnosis. It can help if you deal with panic attacks, depression, self-harm urges, suicidal thoughts, extreme stress, trauma reactions, substance use, or intense mood changes. It can also help if your mental state sometimes changes fast and you need a simple guide that says, "Here is what I do next."
A mental health crisis is a situation where your thoughts, feelings, or behaviors become so intense that your safety, daily functioning, or judgment is seriously affected. A crisis does not always look dramatic. It might be a panic attack that will not stop, several days of not getting out of bed, thoughts of hurting yourself, or feeling so overwhelmed that you cannot trust yourself to stay safe.
Planning ahead matters because a crisis often affects memory, focus, and decision-making. You may forget numbers, downplay danger, avoid reaching out, or convince yourself that no one can help. A plan reduces guesswork. It turns a huge emotional problem into a smaller list of actions: who to contact, what to say, where to go, and how to make the environment safer.
Think of it like having a fire escape plan in your home. You hope you never need it, but if smoke fills the room, that is not the moment to start figuring out the exit. Mental health emergencies work the same way. Fast access to a plan can lower harm and speed up support.
Crisis plan means a written set of steps you will follow if your mental health becomes unsafe or feels out of control. It includes warning signs, coping actions, support people, professional contacts, and emergency steps.
Trigger means a situation, memory, event, or stressor that makes symptoms worse.
Protective factor means something that lowers risk or helps you stay safe, such as a supportive adult, treatment, healthy routines, or access to help.
You do not need a perfect plan. You need a usable one. A short plan you can actually follow is much more helpful than a long document you never open.
Your warning signs are the clues that tell you your mental state is getting worse. They often build in stages, as [Figure 1] shows, starting with early changes and moving toward serious danger if nothing interrupts the pattern. Learning your signs helps you act sooner, when support is easier to use.
Warning signs can be emotional, physical, behavioral, and social. Emotional signs might include feeling numb, hopeless, angry all the time, unusually anxious, or trapped. Physical signs can include sleeping far too little or too much, appetite changes, shaking, stomach pain, headaches, or feeling constantly exhausted. Behavioral signs may include missing responsibilities, not showering, self-harm, impulsive choices, or using substances to cope. Social signs can include isolating, suddenly deleting accounts, posting goodbye messages, or pulling away from people you usually trust.
Pay attention to your digital behavior too. For students who learn online, warning signs may show up in missed logins, ignored messages, camera avoidance during check-ins, disappearing from group chats, doom-scrolling late at night, or posting in ways that suggest despair or danger. Those patterns count. Mental health does not only show up offline.
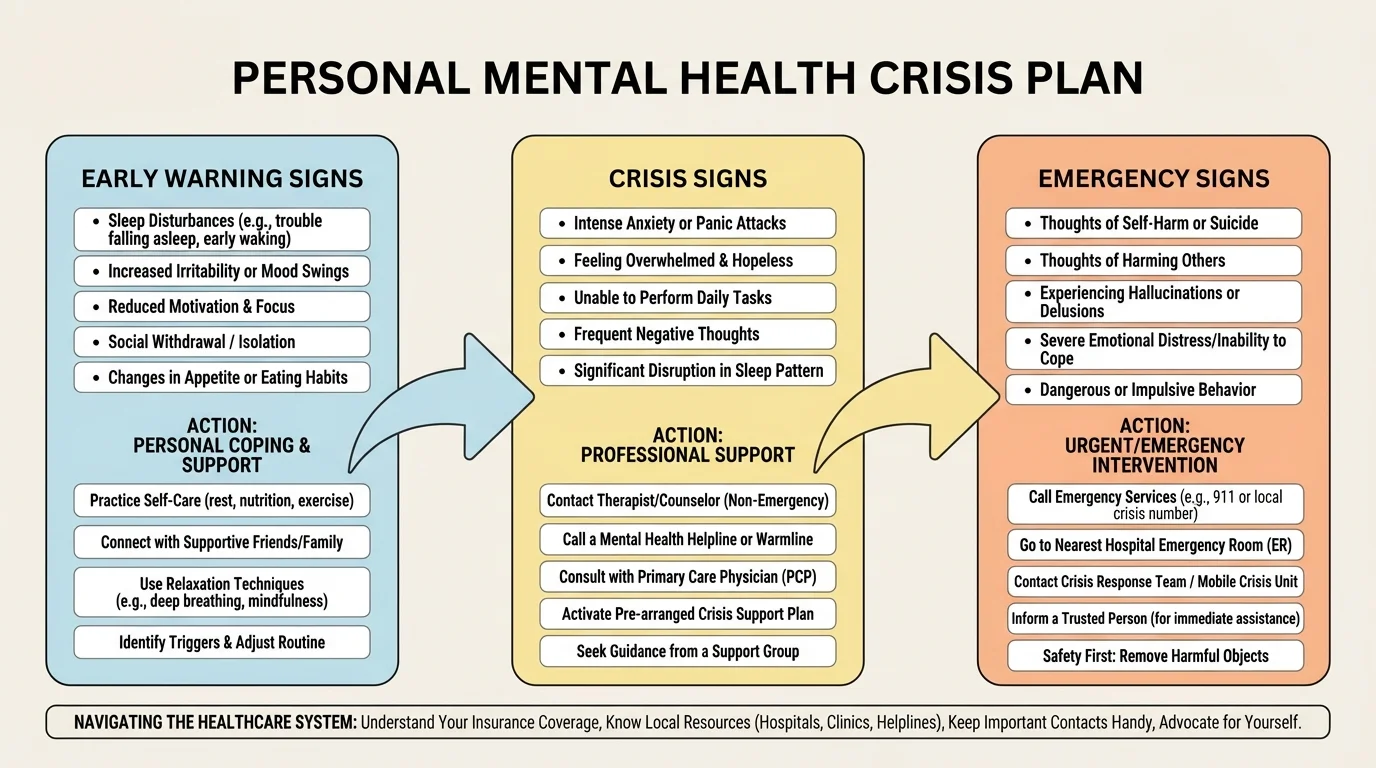
Try to sort your signs into three levels:
Early signs: You are struggling, but still able to function somewhat. Example: you stop replying to friends, sleep badly for several nights, and feel more irritable than usual.
Crisis signs: Your coping is breaking down. Example: you cannot focus, you skip basic care, panic becomes frequent, or you feel like you might do something unsafe.
Emergency signs: Immediate danger is possible. Example: you have a plan to harm yourself, you cannot promise your own safety, you are hearing or seeing things that are not there, or you are so impaired that you cannot stay safe alone.
One useful way to identify warning signs is to look backward. Ask yourself: "When I was having a really hard week, what changed first?" Maybe it was staying up until 2:00 a.m., ignoring texts, eating almost nothing, or thinking "everyone would be better off without me." Those are not random details. They are data about your pattern.
Case study: noticing a pattern early
Jalen starts feeling overwhelmed during a stressful month. Instead of waiting until everything falls apart, he tracks what happens first.
Step 1: He lists early signs.
He notices he stops turning in online assignments, keeps his room dark all day, and sleeps only a few hours.
Step 2: He identifies crisis signs.
He begins having panic attacks, avoids everyone, and thinks, "I cannot do this anymore."
Step 3: He identifies emergency signs.
If he starts thinking about hurting himself or cannot stay safe by himself, that means it is time for immediate outside help.
Because he knows the pattern, he can act at the early-sign stage instead of waiting for an emergency.
The earlier you respond, the more choices you usually have. That is one of the biggest reasons a crisis plan works.
Your plan should be concrete, specific, and easy to skim. A good plan is less like a journal entry and more like a checklist, as [Figure 2] illustrates. If you are shaky, crying, panicking, or exhausted, you need clear instructions, not long paragraphs.
Start with your top warning signs. Keep the list short. Choose the signs that most reliably mean you need to act. For example: "I stop eating regular meals," "I isolate and ignore messages," "I start thinking people would be better off without me," and "I cannot calm down for over an hour."
Next, list your coping strategies. These are actions you can take on your own for short-term stabilization. Good coping strategies are realistic, safe, and specific. "Feel better" is not useful. "Take a shower, drink water, put my phone on do not disturb for 20 minutes, use paced breathing, sit with my dog, and text one trusted person" is useful.
Include only strategies that actually help. If journaling makes you spiral, leave it off. If music helps only sometimes, note what kind. If social media makes things worse, say that clearly. Your plan should be honest, not idealized.
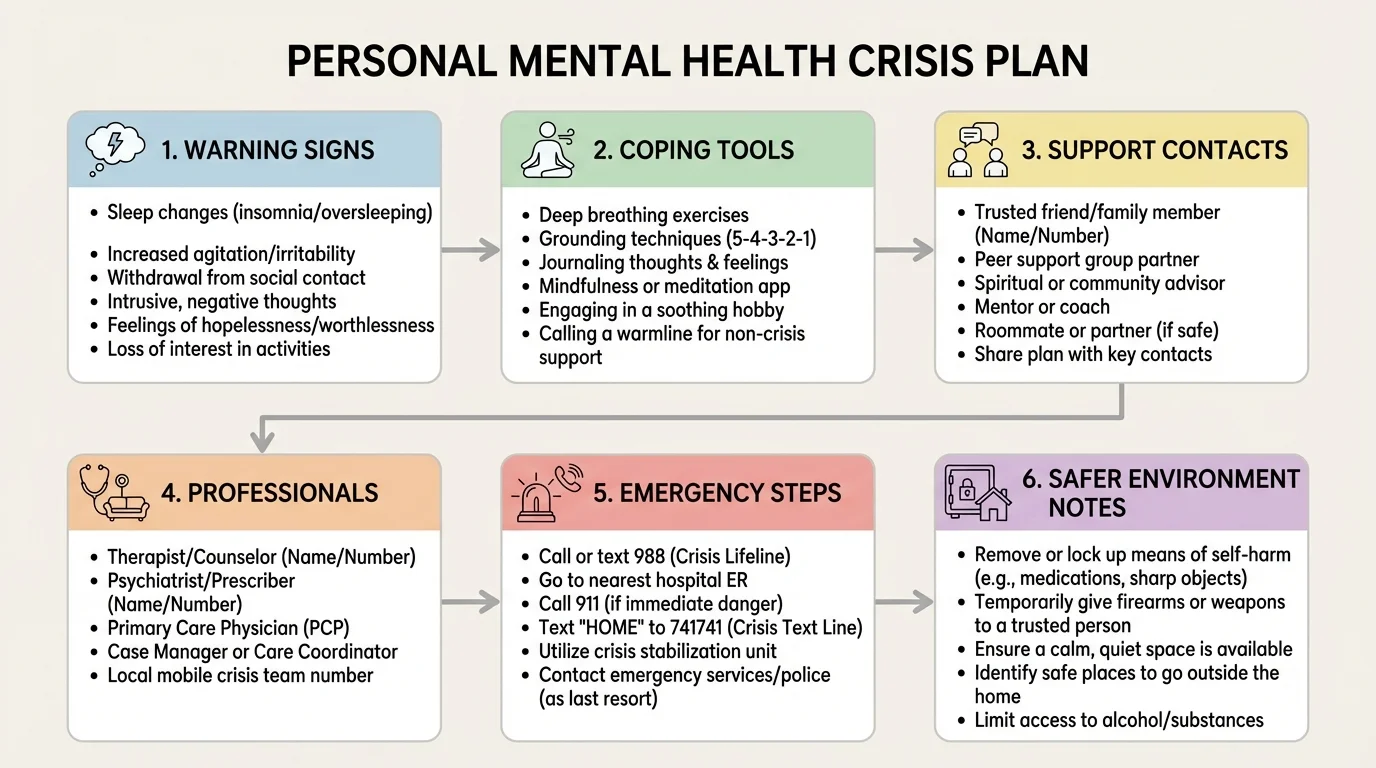
Add a section called People I can contact. Include names, roles, and contact information. Be specific: parent, older sibling, aunt, coach, youth group leader, therapist, doctor, neighbor, family friend. If you tend to freeze when reaching out, write a script such as: "I'm not okay and I need you to stay on the phone with me," or "My warning signs are getting worse and I need help getting professional support today."
Then include professional support information: therapist name, clinic number, psychiatrist if you have one, primary care doctor, local crisis line, and the emergency number for your area. If your location uses a crisis text line or mobile crisis team, include that too. Keep phone numbers accurate and updated.
Your plan should also have a safer environment section. If you are at risk of harming yourself, reducing access to dangerous items matters. That might mean giving medications, sharp objects, cords, firearms, or car keys to a trusted adult, or asking not to be left alone. This step is serious and practical. Safety planning works best when it changes the environment, not just your thoughts.
Finally, include emergency actions. Write exactly what happens if the situation becomes urgent. For example: "If I cannot stay safe, I will tell my mom immediately, call a crisis line, and go to urgent or emergency care. I will not stay alone." This removes the temptation to negotiate with danger.
A strong plan is specific enough to follow under stress. The best crisis plans answer six practical questions: What am I noticing? What can I do right now? Who do I contact first? Which professional support do I use? How do I make the environment safer? What happens if the risk becomes immediate? If your plan answers all six, it is already useful.
Keep your plan to one page if possible. A notes app, printable document, or lock-screen shortcut can all work. The point is access, not appearance.
One reason people delay help is that they think "professional support" means only one thing. It does not. Different professionals do different jobs, and knowing the difference saves time.
A therapist or counselor helps you talk through emotions, patterns, coping, trauma, relationships, and behavior changes. A psychiatrist is a medical doctor who can diagnose conditions, monitor symptoms, and prescribe medication. A primary care doctor can also be a starting point, especially if you do not already have a mental health provider. They can screen for depression, anxiety, sleep problems, substance use, and refer you to specialists.
If you are not sure how to begin, start with one sentence: "I'm concerned about my mental health and I need an appointment." You do not need a perfect explanation. If talking feels hard, write a message or ask a trusted adult to help make the call.
Here are examples of what you can say:
"My anxiety has been getting worse and it is affecting my sleep and schoolwork."
"I have been feeling depressed for weeks and I need support."
"I am having thoughts of hurting myself and I need help right away."
The last example is urgent. If you are in immediate danger, skip routine scheduling and use emergency support.
Many people think they need to wait until things are "bad enough" before asking for help. In reality, getting help earlier often means more choices, shorter recovery time, and less chance of reaching a crisis point.
If you are a teen, access may involve a parent, guardian, or another adult depending on local laws and the kind of treatment. Even when privacy rules vary, safety comes first. If there is serious risk of self-harm, suicide, abuse, or inability to care for yourself, adults and professionals may need to act to protect you.
The mental healthcare system can feel confusing until you sort it by urgency. That is why a step-by-step decision path helps, as [Figure 3] shows. The main question is not "What is the perfect resource?" It is "What level of support do I need right now?"
If your symptoms are uncomfortable but you are safe, routine care is usually the right starting point. That may mean scheduling therapy, contacting your doctor, or asking a trusted adult to help you find a provider. If your symptoms are getting intense fast, you may need same-day support such as a crisis line, urgent behavioral health service, or mobile crisis team if available in your area.
If you are in immediate danger, cannot promise your safety, have taken steps toward suicide, are severely impaired by substances, or are experiencing psychosis or violent impulses, that is emergency-level care. Use emergency services, go to the nearest emergency department, or call the emergency number in your area. Do not stay alone with immediate risk.
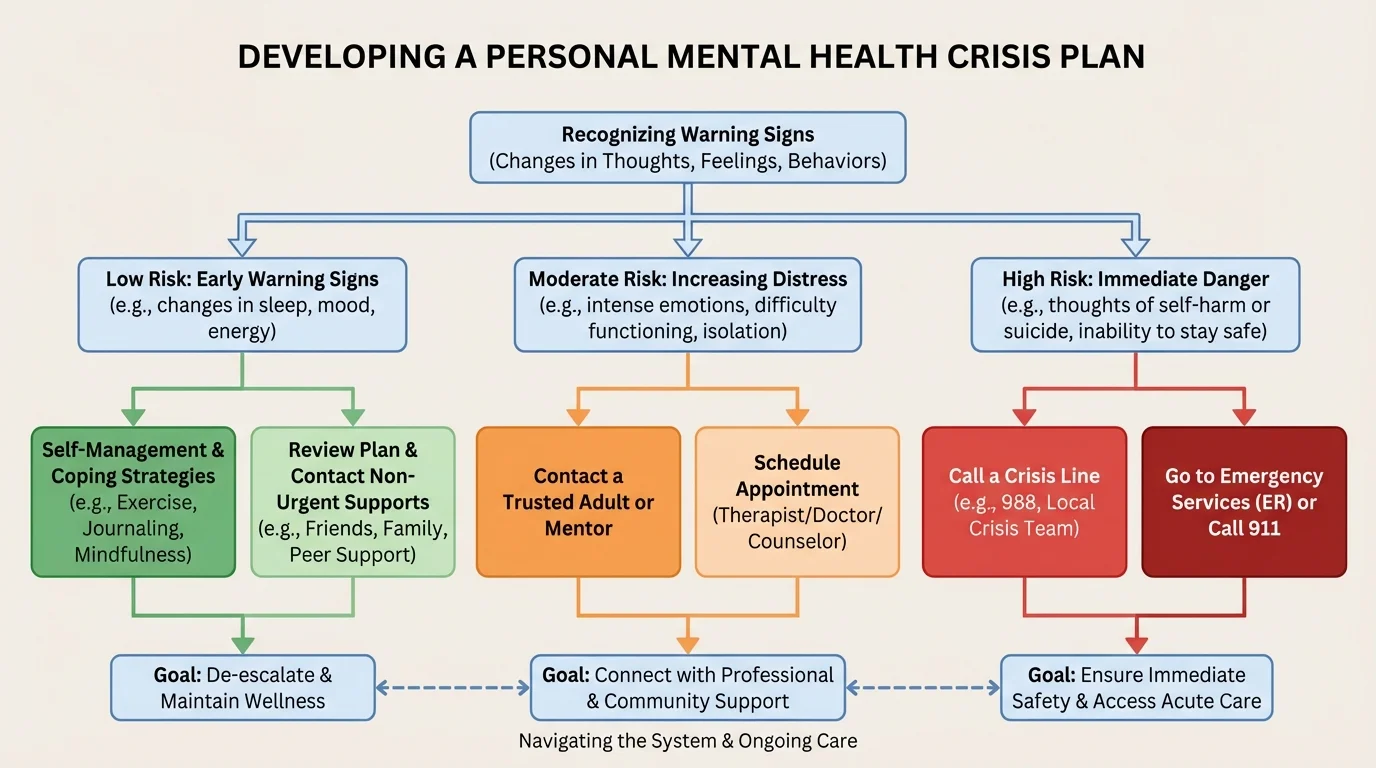
It also helps to understand a few common system terms. Referral means one professional sends you to another provider or service. Intake is the first appointment or screening where they ask questions about your symptoms, history, safety, and goals. Confidentiality means your personal information is protected, though there are safety-related limits when someone may be in danger.
If insurance is part of your family's healthcare, you may hear terms like "in-network" and "copay." In-network usually means the provider has agreed to your insurance plan's rates. A copay is the amount paid at a visit. If your family does not use insurance, there may still be community clinics, community-based youth services, telehealth providers, or sliding-scale counseling with lower fees.
When you contact a provider, ask practical questions: Do you work with teens? Do you treat anxiety, depression, trauma, or self-harm? Do you offer telehealth? What is the wait time? What should I do if things get worse before the first appointment? Those questions help you avoid getting stuck.
| Situation | Best first step | Why |
|---|---|---|
| You feel stressed, anxious, or down, but safe | Schedule a therapist or doctor visit | Routine care can address problems before they grow |
| Your symptoms are worsening quickly | Tell a trusted adult and contact urgent support | Fast help can prevent an emergency |
| You have thoughts of self-harm or suicide | Use a crisis line, trusted adult, or emergency support immediately | Safety takes priority over privacy or embarrassment |
| You cannot stay safe alone | Go to emergency care or call emergency services | Immediate danger needs immediate protection |
Table 1. A practical guide to matching mental health situations with the right level of support.
Notice that embarrassment is never a good reason to avoid care. Many people worry they are "overreacting." If safety is uncertain, it is better to reach out and be safe than stay silent and get worse.
A plan only works if you know how to activate it. The first rule is simple: use it when warning signs start, not only when things become unbearable. That is why early signs in [Figure 1] matter so much. They are your signal to stop, check the plan, and take the first action.
Suppose your anxiety spikes after a conflict online. Your chest feels tight, you cannot stop replaying the messages, and you want to disappear from every app. The plan might tell you to log off, drink water, do paced breathing for a few minutes, contact one safe person, and avoid being alone until you settle. If the panic keeps climbing, the next step might be contacting a parent or calling a support line.
Or maybe depression has been building for two weeks. You are sleeping all day, missing classes, and thinking that nothing matters. Your plan may say: tell one adult today, book an appointment, eat one simple meal, move to a shared room instead of isolating, and hand over anything you could use to hurt yourself if those thoughts are present.
If suicidal thoughts become specific, frequent, or connected to a plan, that is no longer a "wait and see" situation. Use the emergency steps exactly as written. Tell an adult clearly, do not stay alone, and use emergency or crisis services. Your safety matters more than keeping the moment quiet.
Real-life script for asking for help
If words disappear when you are overwhelmed, use a script you already saved.
Step 1: State the problem clearly.
"I am having a mental health crisis and I do not feel safe handling it by myself."
Step 2: Say what you need next.
"I need you to stay with me and help me contact support."
Step 3: Add urgency if needed.
"This is urgent. I am having thoughts of hurting myself."
Short, direct language gets faster results than trying to sound calm or minimize what is happening.
If you are worried about a friend, take it seriously. You do not have to become their counselor. Your job is to connect them with real help. If a friend says they want to die, might hurt themselves, or cannot stay safe, involve a trusted adult and emergency support right away. Keeping a dangerous secret is not loyalty. It can be deadly.
"Asking for help is a safety skill, not a weakness."
That is especially true in online life. If a friend posts a goodbye message, sends alarming texts, or suddenly talks as if they are done with everything, respond, but also escalate. Contact a trusted adult, parent, guardian, crisis service, or emergency support. Do not carry that alone.
A crisis plan is not something you write once and forget. It should change as you learn more about yourself. As you saw in [Figure 2], the strongest plans are built from real patterns and real supports, so update yours whenever those change.
Review your plan every few months, after a hard episode, after starting or stopping treatment, or whenever your supports change. Check that the contacts are current. Make sure the coping steps still help. Remove anything unrealistic and add anything that has worked.
Store the plan where you can reach it fast: in your phone notes, a shared family document, a printed copy near your desk, or a small card in your wallet. If you trust certain adults, share the plan with them. It is easier for someone to help you if they already know your warning signs and your preferred next steps.
Try this: spend 15 minutes creating a first draft today. You do not need every detail finished. Start with three warning signs, three coping actions, two trusted people, one professional contact, and one emergency step. That draft is already better than having no plan at all.
Another smart move is practicing one part of the plan while you are calm. Save support numbers, type a help message draft, or tell a trusted adult, "If I text you this phrase, it means I need help right away." Small preparation makes action easier under pressure.
Your plan is personal, but it should never depend only on willpower. Safe people, professional support, and environmental safety steps are just as important as coping tools.
If your plan ever feels too heavy to make alone, build it with an adult, therapist, doctor, or counselor. You are allowed to need help creating a help plan.