One of the fastest ways to feel like an adult is also one of the least glamorous: handling your own health. No one posts about finally calling a doctor's office, checking whether a symptom needs urgent care, or remembering to refill a prescription before it runs out. But these are exactly the kinds of decisions that affect whether you stay safe, miss work, lose money, recover quickly, or let a small problem become a serious one.
Health management is not just "going to the doctor when something feels wrong." It includes sleep, food, movement, stress, medication safety, access to care, digital privacy, emergency planning, and knowing when to ask for help. As you take on more adult responsibilities, you also take on more responsibility for tracking your body, your symptoms, your appointments, and your choices.
As a child, someone else may have scheduled checkups, kept insurance cards, noticed refill dates, or decided whether your fever needed a clinic visit. As you become more independent, those tasks start shifting to you. That shift matters because adult life often gives you more freedom, but it also gives you more chances to ignore warning signs, delay treatment, or make risky choices.
Good health management means you can function in daily life. If you sleep enough, eat regularly, stay hydrated, manage stress, and get help when needed, you are more likely to work well, drive safely, think clearly, and handle relationships responsibly. Poor health management has real consequences: missed deadlines, worsened illness, avoidable bills, medication mistakes, burnout, and dangerous emergencies.
Health management as a life system
Think of health management as a system, not a one-time action. A system includes prevention, noticing problems early, choosing the right type of care, following instructions, and protecting yourself in emergencies. The goal is not perfection. The goal is to make safe, informed choices consistently enough that your health supports the life you want to build.
A practical mindset helps: instead of waiting until things get bad, you learn to ask, What do I need right now, what can wait, and who can help? That question applies to a sore throat, an anxiety spike, a sports injury, a late-night ride home, or a medication refill.
Before you can manage your health well, you need to know your own basic information. This includes your full legal name, date of birth, address, emergency contact, allergies, current medications, past major illnesses or injuries, and any conditions a doctor should know about. If you cannot quickly answer those questions, start collecting the information now.
Your medical history is the record of past illnesses, surgeries, injuries, conditions, and family health patterns that may affect your care. You do not need to memorize every detail, but you should know the big things: asthma, diabetes, severe allergies, prior concussions, mental health diagnoses, past hospitalizations, and medicines you take regularly or recently stopped.
You should also know if you have any allergies, especially to foods, medications, latex, or insect stings. A mild preference is not the same as an allergy. If a substance causes hives, swelling, breathing trouble, or a severe reaction, that information needs to be easy to access.
Primary care is routine medical care from a primary care doctor or nurse practitioner who helps with checkups, common illnesses, prevention, and ongoing health concerns.
Telehealth is healthcare provided remotely by phone or video for concerns that do not require hands-on treatment.
Urgent care treats problems that need quick attention but are not life-threatening.
Emergency room care is for severe or potentially life-threatening situations that need immediate treatment.
Keep a basic health note on your phone or in a secure document. Include your pharmacy, any prescriptions, insurance information if you have it, and an emergency contact. If you use a wallet, keep a physical card with your name, emergency contact, allergies, and medications. This is especially important if you drive, travel alone, play sports, or work outside the home.
If you are covered by health insurance, learn the basics of your card. Know the member ID, the plan name, and whose plan it is. You do not need to become an insurance expert today, but you should recognize the card, know how to present it, and understand that in-network care is usually less expensive than out-of-network care.
One of the most useful adult skills is knowing triage: deciding how urgent a problem is and what level of care fits it. Choosing well saves time, money, and stress. If you use the emergency room for a minor issue, you may wait a long time and pay more than necessary. If you ignore a serious symptom, the risk can be much worse.
[Figure 1] Use self-care at home for mild problems you understand and can safely monitor, such as a minor headache improved by rest, slight muscle soreness after exercise, or a small scrape that you can clean and bandage. Use reliable guidance from a trusted healthcare source, not random social media advice.
Use primary care for checkups, vaccines, non-urgent illness, ongoing issues like recurring headaches, questions about nutrition or sleep, and follow-up on chronic concerns. Use telehealth for things like medication questions, mild illness, some mental health support, or advice when you are unsure whether you need in-person care.
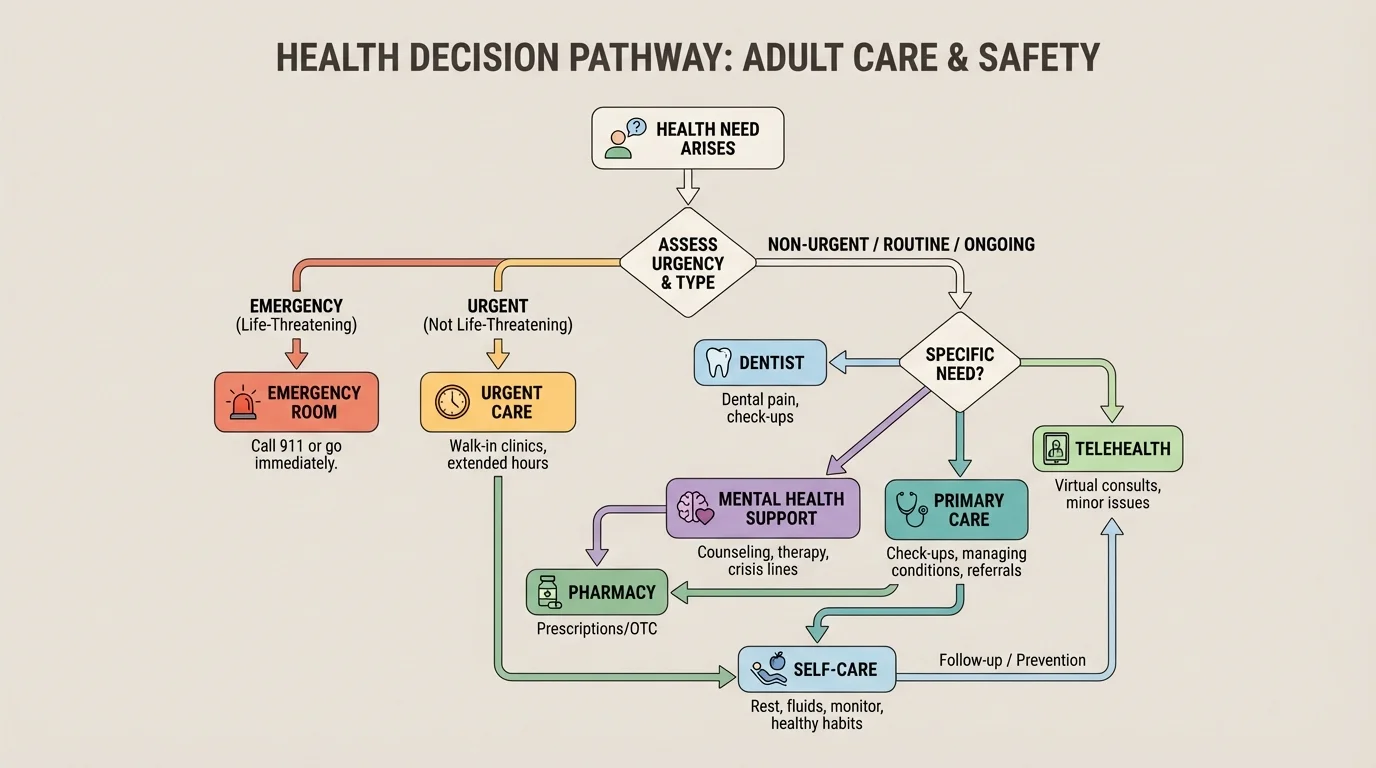
Use urgent care for problems that should be treated soon but are not immediately life-threatening: a possible sprain, a fever that will not come down, painful ear infection symptoms, a cut that may need stitches, or worsening flu-like symptoms. Use the emergency room or call emergency services for chest pain, severe trouble breathing, symptoms of stroke, major head injury, heavy bleeding, a seizure, loss of consciousness, severe allergic reaction, or signs that someone may harm themselves or others.
Not every problem belongs to a doctor's office. A dentist handles tooth pain, gum swelling, or broken teeth. A pharmacy can help with prescription refills, over-the-counter medications, and questions about safe medication use. A licensed therapist, counselor, psychiatrist, or crisis service may be the right support for panic attacks, depression, persistent anxiety, trauma symptoms, or thoughts of self-harm.
Later, when you are deciding between options under stress, the pattern in [Figure 1] stays useful: start by asking whether the issue is mild, urgent, or dangerous, and then match the care setting to the need.
Many people delay care because they are afraid of "bothering" a professional or sounding dramatic. In reality, health systems expect people to ask questions. Getting guidance early often prevents a much bigger problem later.
A good rule is this: if you are unsure and symptoms are severe, fast-changing, or affecting breathing, consciousness, or safety, treat the situation as urgent and seek immediate help. It is better to be checked and told you are okay than to gamble with a serious condition.
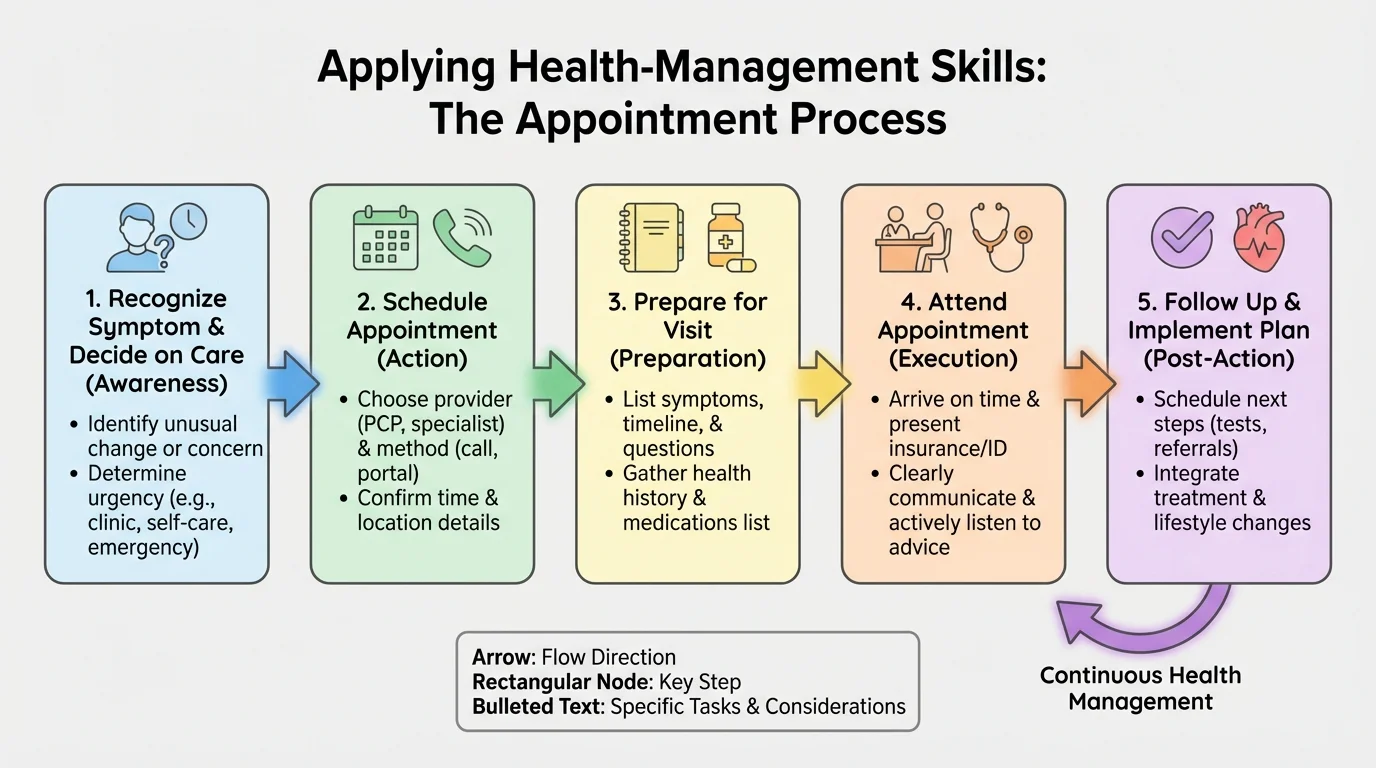
Appointments go much better when you use a repeatable process. Adult health management is not about sounding impressive. It is about giving clear information: what you feel, when it started, what makes it better or worse, and what you need help understanding.
[Figure 2] When you make an appointment, be ready to share your name, date of birth, phone number, insurance information if needed, and a brief reason for the visit. Keep the reason short and specific. "I've had a sore throat and fever for two days" works better than a long story. If the problem involves safety, say so clearly: "I'm having severe pain," "I'm struggling with panic and can't calm down," or "I think I may have a concussion."
Before the visit, write down your symptoms. Note when they started, how often they happen, how strong they are, and anything that seems connected. If pain matters, rate it on a scale of \(0\) to \(10\), where \(0\) means no pain and \(10\) means the worst pain you can imagine. Also list medications, supplements, allergies, temperature readings if relevant, and questions you do not want to forget.
Bring what you need: your phone, ID if required, insurance card if you have one, payment method if needed, and your notes. If the appointment is virtual, test your internet, microphone, and camera a few minutes early. Find a private, quiet place so you can speak honestly.
Example: Preparing for a doctor visit about recurring headaches
Step 1: Track the pattern
You notice headaches on \(4\) days this week, mostly after sleeping only \(5\) to \(6\) hours and skipping breakfast.
Step 2: Write a clear reason for the visit
"I've had recurring headaches for about \(3\) weeks. They happen several times a week and sometimes make it hard to focus."
Step 3: Prepare questions
Ask: "Could this be related to sleep, screen time, dehydration, stress, or vision?" and "What warning signs would mean I need urgent care?"
Step 4: Follow the plan after the visit
If you are told to increase water, improve sleep, reduce caffeine, and book an eye exam, put those actions in your calendar instead of trusting yourself to remember.
This kind of preparation helps the professional give you better care faster.
During the visit, answer honestly. If you smoke, vape, drink, use drugs, have sex, skip meals, or avoid sleep, that information can affect your care. Health professionals are there to treat you, not to reward you for looking perfect. If you do not understand a term or instruction, ask for plain language. Say, "Can you explain that another way?" or "What should I do first when I get home?"
After the appointment, follow-up matters. Read the visit notes if you receive them. Pick up the medication. Schedule the test. Set the reminder. If symptoms get worse or the plan is not working, contact the office again. A treatment plan only helps if you actually use it.
As you build confidence, the sequence shown in [Figure 2] becomes automatic: notice, record, book, prepare, attend, and follow through.
Independent health is easier when you do not live in emergency mode. Prevention is not dramatic, but it is powerful. Basic habits lower risk, improve mood, and make it easier to notice when something is wrong because your normal baseline is more stable.
Your preventive care includes checkups, vaccines, dental visits, sleep, hydration, balanced eating, movement, stress reduction, and safer choices around sex and substances. Prevention does not guarantee perfect health. It improves the odds and helps problems get caught earlier.
Sleep is a safety issue, not just a comfort issue. Too little sleep affects mood, memory, reaction time, and decision-making. If you drive while exhausted, your risk increases. If you work, study, exercise, or manage conflict while severely sleep-deprived, you are more likely to make mistakes.
Nutrition and hydration matter for energy, concentration, and recovery. You do not need a perfect diet to take care of yourself. You do need enough fuel. Skipping meals regularly, relying only on energy drinks, or forgetting water can lead to headaches, irritability, fatigue, and poor focus.
Movement supports health even when life is busy. This does not have to mean intense workouts. Walking, stretching, bodyweight exercises, sports, dancing, and active commuting can all count. The practical goal is consistency.
Healthy routines are most effective when they are realistic enough to repeat. A simple routine you follow most days is more useful than an ideal routine you abandon after a week.
Mental health prevention matters too. Pay attention to patterns: trouble sleeping, withdrawing from people, constant irritability, panic, loss of interest, or feeling hopeless. Those are signs to take seriously, not personality flaws to hide. Reaching out early can prevent a deeper crisis.
Sexual health is part of adult health management. That includes consent, contraception, testing when appropriate, and knowing that embarrassment is not a reason to avoid accurate information or medical care. Safer choices protect both you and other people.
Medication adherence means taking medicine exactly as directed: the right amount, at the right time, for the right length of time. Stopping antibiotics early because you "feel better," doubling a dose because you missed one, or sharing prescription medication with someone else can be unsafe.
| Health area | Low-effort adult habit | Why it matters |
|---|---|---|
| Sleep | Set a consistent sleep window | Improves focus, mood, and safety |
| Hydration | Carry a water bottle and refill it | Helps energy and reduces headaches |
| Medication | Use phone reminders | Prevents missed doses and refill gaps |
| Dental care | Schedule regular cleanings | Prevents pain and expensive treatment |
| Mental health | Check in on stress weekly | Helps you act before burnout grows |
| Safety | Keep emergency contacts updated | Saves time in urgent situations |
Table 1. Practical health-management habits that are easy to maintain and have strong real-world benefits.
Health management also means protecting yourself before a crisis starts. Emergency preparation is easiest when done in advance. In a real emergency, people forget details, lose time, and panic. Systems reduce that risk.
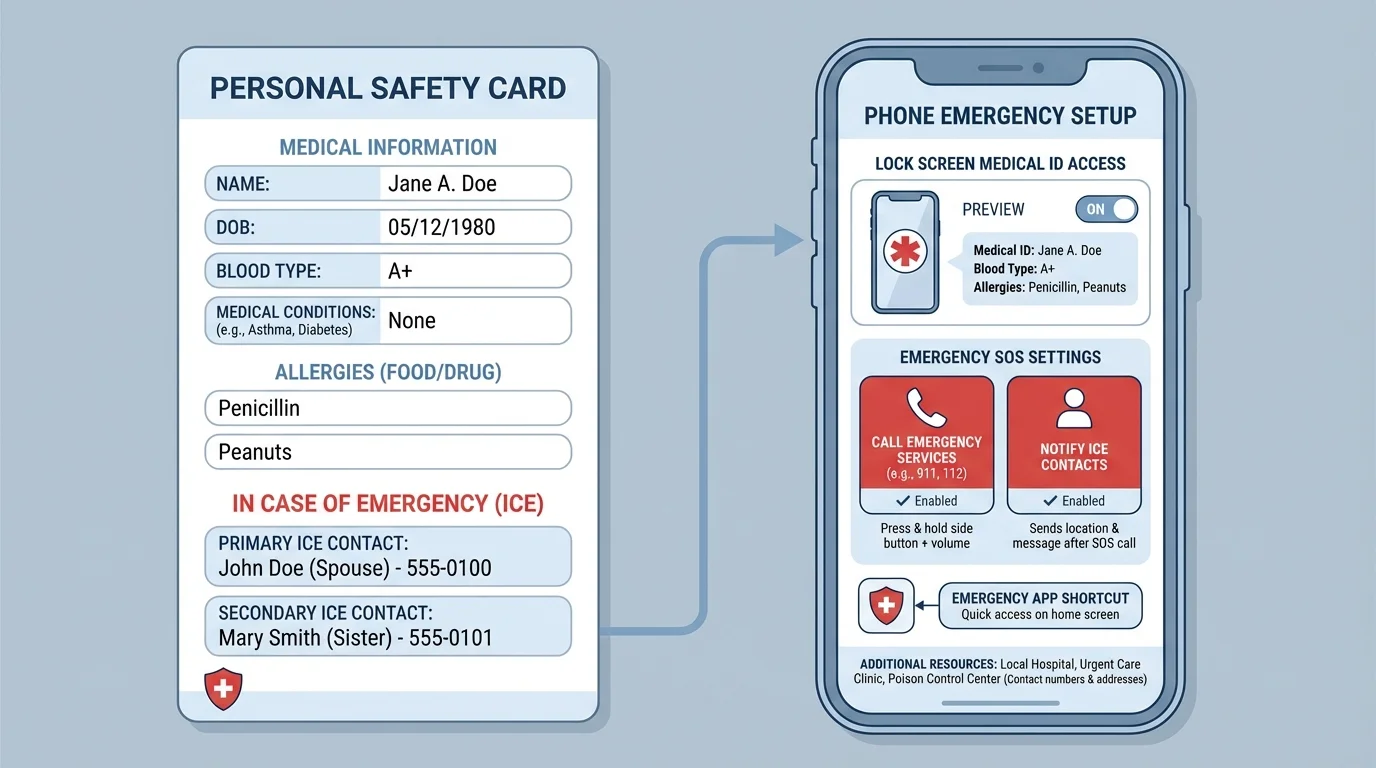
[Figure 3] Start with the basics. Save emergency contacts in your phone. Add an ICE contact, which stands for In Case of Emergency contact. Learn your address and any access details someone might need if help is coming to your location. If you have major allergies, important medications, or a significant condition, keep that information accessible.
Know the warning signs that require immediate action: difficulty breathing, severe allergic reaction, suicidal thoughts with immediate danger, chest pain, heavy bleeding, overdose, seizure, or someone not waking up. In those moments, your job is not to be calm and impressive. Your job is to get help fast.
Home safety matters too. Store medications where children, pets, or visitors cannot casually access them. Check expiration dates. Never mix medications without checking instructions. Use smoke detectors, lock doors and windows, and know basic fire and exit planning. If you live or stay with others, make sure everyone knows what to do if there is a medical emergency.
Substances can turn ordinary mistakes into emergencies. Alcohol, cannabis, nicotine products, vaping, and other drugs can affect coordination, reaction time, mood, and judgment. Mixing substances or using them with medications can increase risk. Never get in a car with an impaired driver, and do not assume someone is "fine" just because they are acting confident.
Consent and personal safety belong in this conversation too. If a situation feels coercive, unsafe, or hard to leave, pay attention to that feeling. Protecting your health includes protecting your boundaries. Let trusted people know where you are, arrange your own transportation when possible, and have an exit plan.
Your digital life can affect your physical safety. Protect health portals, insurance accounts, and pharmacy logins with strong passwords and two-factor authentication. Be cautious about posting your location live or sharing private medical information casually online. Once private information spreads, you may not be able to control where it goes.
When a real emergency happens, the preparation in [Figure 3] saves time: key details are already organized, contacts are ready, and you are less likely to freeze.
"The best emergency plan is the one you set up before you need it."
A strong system does not have to be complicated. It just has to be reliable. Start by choosing one place to keep health information: a secure notes app, a folder, or both digital and paper copies. Include your insurance information, medications, allergies, doctor and dentist contact information, and dates of recent appointments.
Then build reminders. Put annual checkups, dental cleanings, medication refills, and vaccine records somewhere you already check, such as your calendar app. If a prescription lasts \(30\) days, do not wait until day \(30\) to refill it. Set a reminder around day \(25\) so you have time if the pharmacy is delayed.
Use a simple weekly reset. Ask yourself: Do I need to refill anything? Have I been sleeping enough? Am I ignoring a symptom? Do I know my schedule well enough to book care without waiting until the problem gets worse? Five minutes of review can prevent a messy week.
Example: A basic personal health system
Step 1: Create one health note on your phone
List medications, allergies, pharmacy, doctor, dentist, and emergency contacts.
Step 2: Add reminders
Use calendar alerts for medication refill dates, appointments, and annual checkups.
Step 3: Keep a symptom log when needed
If something repeats, record dates, triggers, and severity instead of relying on memory.
Step 4: Review weekly
Take a few minutes every week to check whether anything needs attention before it becomes urgent.
This system is simple, but it helps you act earlier and with less stress.
You can also build support into your system. Being independent does not mean handling everything alone. It means knowing when to ask for a parent, guardian, roommate, partner, friend, mentor, pharmacist, nurse line, or clinician. Smart adults use support networks.
Suppose you twist your ankle stepping off a curb. It hurts, but the bone is not sticking out, you can move your toes, and the swelling starts gradually. This may fit home care first or urgent care if you cannot bear weight, swelling grows, or pain is significant. You would rest, ice, elevate, avoid unnecessary strain, and monitor whether symptoms improve.
Suppose you have been feeling anxious for weeks, your sleep is getting worse, and you are avoiding normal responsibilities. This is not something to dismiss as being "bad at coping." It is a reason to contact a mental health professional, primary care provider, or telehealth service. If you are in immediate danger of harming yourself, seek emergency help right away.
Suppose you realize on Sunday night that you have one pill left of a daily prescription. A good system would have caught this earlier, but now you need to act fast: check refill options in the pharmacy app, call the pharmacy, contact the prescriber if needed, and avoid skipping or changing the dose on your own unless instructed.
Suppose a friend becomes hard to wake up after drinking or using substances. This is not a "wait and see" situation. Call emergency services. Keep the person on their side if needed, stay with them, and do not assume sleep and unconsciousness are the same thing.
People often think adulthood means never needing guidance. In reality, adult competence usually looks like noticing a problem early, asking the right questions, and taking action before things spiral.
You do not need to know everything about healthcare to manage your health well. You do need a few reliable habits: notice changes, know your basics, choose the right care, ask clear questions, follow instructions, and protect your safety. Those skills build over time.
Try this: today, save your emergency contact, write down your medications and allergies, and identify one clinic, one pharmacy, and one trusted emergency resource you could use if needed. Then set one health reminder you have been putting off. Small actions are what make independence real.
The goal is not to become fearless. The goal is to become prepared. When you can manage your health responsibly, you protect your future choices, your work, your relationships, and your daily life.