Sometimes the biggest danger is not a dramatic crisis everyone can see. It is the quiet message that goes unanswered, the friend who suddenly disappears from chats, or the thought in your own mind that says, just get through today and then keeps getting darker. Knowing how to recognize severe mental health distress is a real-life safety skill. It can protect your life, support someone you care about, and help you act early instead of waiting until things get worse.
If you learn online, a lot of your social life may take place through text messages, gaming, group chats, video calls, social media, clubs, sports, work, faith communities, or family connections. That means warning signs may show up differently than people expect. You might not see someone face-to-face every day, but you can still notice major changes in mood, behavior, energy, or communication. You can also notice those changes in yourself.
Mental health struggles are common, and many people go through periods of anxiety, sadness, stress, or burnout. That does not automatically mean someone is in immediate danger. But severe distress is different. Severe distress means a person is struggling so much that their safety, daily functioning, judgment, or hope is seriously affected. When that happens, the right response is not to ignore it, joke about it, or assume it will pass on its own. The right response is to get support.
One reason people miss warning signs is that they expect a crisis to look obvious. In real life, it may look like someone sleeping all day, not replying for long periods, posting hopeless messages, talking about being a burden, giving away belongings, self-harming, taking dangerous risks, or saying they do not want to be here anymore. It may also look like a person who seems unusually calm after a period of intense distress, especially if they have already decided to hurt themselves. That is why paying attention matters.
Severe mental health distress is a level of emotional or psychological suffering that strongly interferes with safety, daily life, or the ability to cope. Help-seeking means reaching out to an appropriate source of support, such as a trusted adult, counselor, doctor, crisis line, or emergency service. Crisis is a situation where someone may be at immediate risk of harming themselves or others, or is unable to stay safe without urgent help.
Recognizing distress is not about labeling people or trying to diagnose them. You are not expected to be a therapist. Your job is simpler and more important: notice serious signs, take them seriously, and connect the person to real help.
Everyone has rough days. You might feel stressed before exams, irritated after poor sleep, or low after an argument. Severe distress is different because it tends to be intense, persistent, or dangerous. It affects basic functioning: sleeping, eating, concentrating, responding to messages, keeping up with responsibilities, or staying safe.
A useful way to think about it is this: ask whether the feeling or behavior is changing how the person lives. Are they isolating much more than usual? Are they acting in ways that scare you? Are they talking as if nothing will ever get better? Are they losing interest in everything, including things that normally matter to them? Are they unsafe right now? If the answer is yes, do not minimize it.
Stress vs. severe distress
Ordinary stress usually rises and falls with a situation and can improve with rest, support, and problem-solving. Severe distress lasts longer, feels harder to control, and may involve hopelessness, panic, self-harm, suicidal thoughts, or major behavior changes. The practical takeaway is simple: if safety, functioning, or hope is seriously dropping, move from "I'll wait and see" to "I need to tell someone and get help."
Another important point: distress can look different in different people. One person may cry and ask for help. Another may become numb, angry, sarcastic, reckless, or silent. Some people post clear warning signs online. Others hide their distress. Because of that, pay attention to patterns and changes, not just stereotypes.
Severe distress often shows up across emotions, behavior, body signals, and online habits, as [Figure 1] illustrates. If several signs are happening at once, especially over days or weeks, that is a strong signal that you should reach out for help rather than trying to manage everything alone.
You may notice emotional signs first: feeling hopeless, trapped, numb, panicked, overwhelmed, constantly on edge, or unusually angry. You might feel like nothing matters, like you are a burden, or like people would be better off without you. Those thoughts are serious warning signs, not something to brush off.
Behavioral signs matter too. You may stop replying to people, avoid calls, stay in bed for long stretches, lose interest in activities you usually care about, fall far behind on responsibilities, use alcohol or drugs to cope, self-harm, or take risks you normally would not take. A sudden drop in self-care can also be a sign.
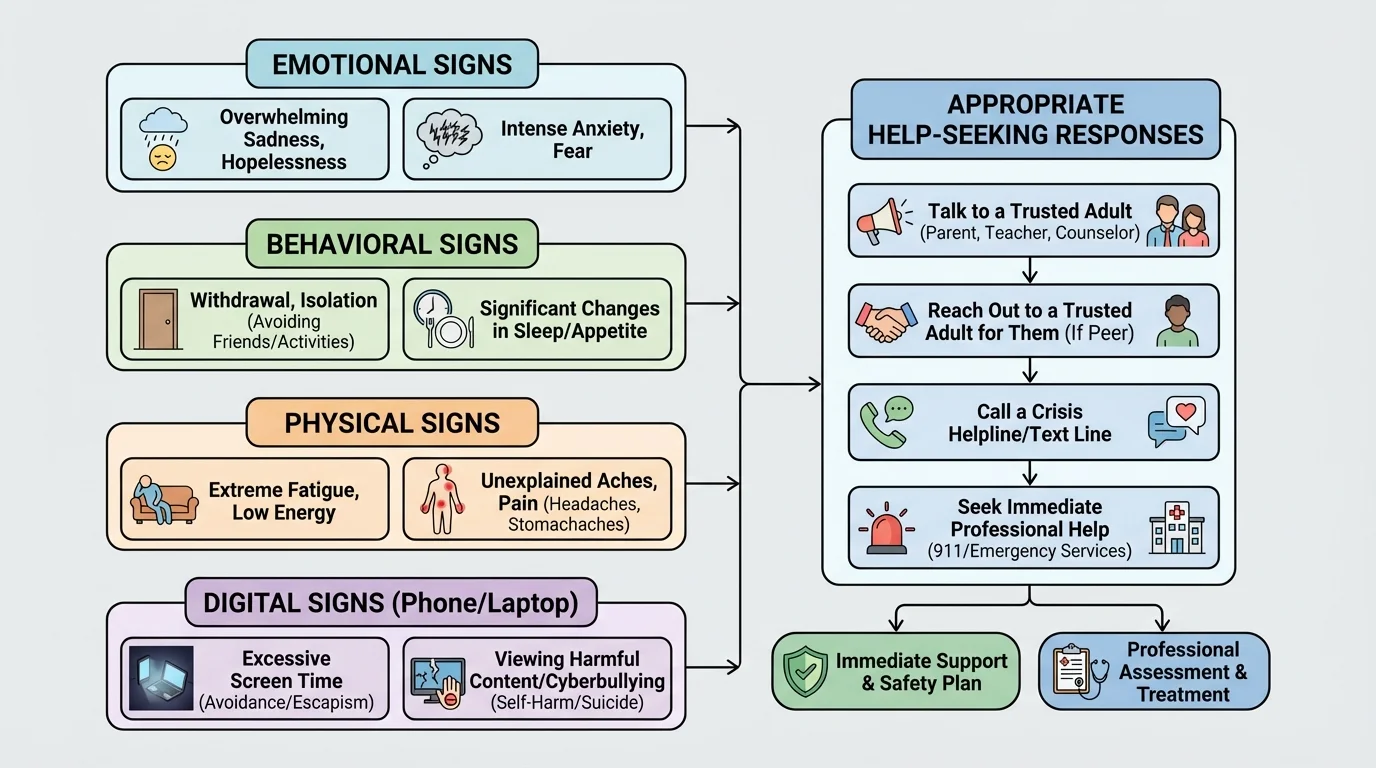
Physical signs can include major sleep changes, appetite changes, exhaustion, agitation, headaches, stomach problems, or feeling physically heavy all the time. These signs do not prove a mental health crisis by themselves, but they matter when they come with emotional pain or major changes in behavior.
In online life, warning signs may include deleting accounts suddenly, posting messages about hopelessness, saying goodbye in a way that feels unusual, withdrawing from group chats, sending alarming late-night messages, searching for harmful content, or writing things like "I'm done," "No one would care," or "I can't do this anymore." When you see a pattern like that in yourself, take it seriously.
If you catch yourself thinking about self-harm or suicide, or planning how you might do it, that moves beyond "I'm struggling" into "I need immediate support." This is especially true if you have access to means, such as medications, weapons, sharp objects, or another specific method. At that point, safety comes first.
You may not know exactly what is happening in another person's life, but you can still notice major changes. A peer might stop logging into social spaces they usually enjoy, leave messages on read for days, start posting dark or hopeless content, sound flat or disconnected on video calls, or say things that suggest they have given up.
Listen for phrases that may signal danger. These include "I can't do this anymore," "Everyone would be better off without me," "Nothing matters," "I just want it all to stop," or "Soon it won't be a problem." Even if the person says it like a joke, do not assume it means nothing.
Also notice sudden changes in personality or routine. Someone who is usually engaged may become unreachable. Someone who is usually careful may suddenly act recklessly. Someone who has been deeply upset may become strangely calm after talking about ending things. As with the pattern in [Figure 1], it is often the combination of signs that matters most.
People often avoid asking directly about suicide because they fear it will "put the idea in someone's head." Research does not support that fear. A calm, direct question can reduce isolation and help a person feel seen.
One more thing: trust your instincts. If something feels seriously off, it is better to check in and involve a responsible adult than to stay silent because you are afraid of overreacting.
Not every painful moment is an emergency, but some situations need fast action. A practical way to respond is to think in three levels, as [Figure 2] shows: concern, serious concern, and emergency.
Concern means something is clearly wrong, but there is no sign of immediate danger. Examples: ongoing sadness, major stress, withdrawal, anxiety, or big changes in sleep and motivation. This still matters. The response is to talk to a trusted adult or mental health professional soon, not weeks later.
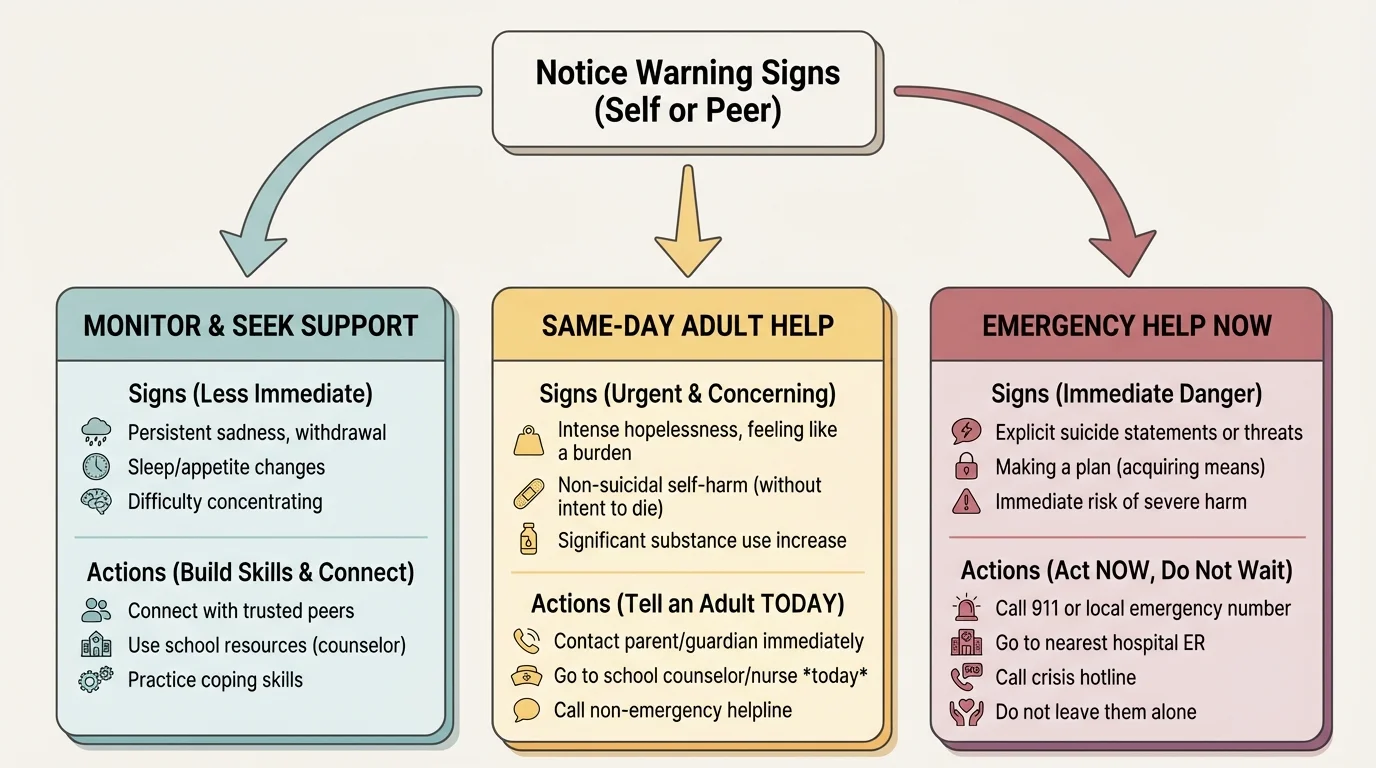
Serious concern means risk is higher and help should happen the same day. Examples: talking about hopelessness, saying they are a burden, self-harming, using substances to cope, looking for ways to die, or saying they do not want to be alive. The response is to tell a trusted adult immediately and stay connected with the person until support is involved.
Emergency means immediate danger. Examples: the person says they are about to hurt themselves, has a plan and access to means, has taken an overdose, is actively self-harming in a life-threatening way, is threatening serious harm to someone else, or cannot stay safe. The response is to call emergency services or a crisis line right away and alert a nearby responsible adult immediately.
| Risk level | What it may look like | Best response |
|---|---|---|
| Concern | Ongoing sadness, withdrawal, anxiety, burnout | Reach out and connect them to support soon |
| Serious concern | Hopelessness, self-harm, suicide talk, dangerous coping | Tell a trusted adult the same day |
| Emergency | Plan, means, attempt, immediate intent, inability to stay safe | Contact emergency services or crisis support now |
Table 1. A practical guide to matching warning signs with the urgency of response.
If you are ever unsure whether something counts as an emergency, choose safety. It is better to get help and find out the risk was lower than to stay silent during a real crisis.
When you are in severe distress, your brain may tell you to hide it, delay, or convince yourself that you are being dramatic. That is the distress talking. Help-seeking is not weakness. It is a safety decision.
Step 1: Name what is happening clearly. Try a sentence like, "I am not okay, and I do not feel safe handling this alone," or "My thoughts are getting scary." Clear language helps you move from vague fear to action.
Step 2: Contact a trusted adult. This could be a parent, guardian, relative, coach, club leader, supervisor, family friend, counselor, doctor, or another responsible adult. If the first person does not respond, contact the next one. Keep going until you reach someone.
Step 3: Be direct. You do not need a perfect explanation. You can say, "I think I need mental health help," "I have been having thoughts of hurting myself," or "I don't feel safe being alone right now." Direct words get faster support.
A practical help-seeking script for yourself
If speaking feels hard, send a short message and then follow up with a call if you can.
Step 1: Start with urgency
"I need help right now with my mental health."
Step 2: Say what the risk is
"I'm having thoughts about hurting myself," or "I don't feel safe being alone."
Step 3: Ask for a clear action
"Can you stay on the phone with me and help me get support?"
Short, clear messages are often more effective than trying to explain everything at once.
Step 4: Reduce immediate danger if possible. Move away from anything you could use to harm yourself. Go where other safe people are. Hand medications, sharp objects, cords, or other dangerous items to an adult if you can. If you cannot keep yourself safe, contact emergency services or a crisis line immediately.
Step 5: Stay connected until help is in place. Do not make a private deal with yourself to wait it out alone. If your thoughts are becoming more intense, tell someone that clearly.
Try This: Save at least three support contacts in your phone under names you will recognize quickly, such as "Mom," "Uncle Jay," or "Crisis Help." Also write a short emergency text now, before you need it. When people are overwhelmed, prewritten words can make action easier.
Helping a friend works best when you follow a clear sequence of actions, as [Figure 3] illustrates. Your role is to notice, check in, ask about safety, and connect them with real help. Your role is not to become their only support or to carry a crisis by yourself.
Start by checking in directly and calmly. Instead of hinting, say what you noticed. "You haven't been yourself lately," "Your posts sound really hopeless," or "I'm worried because you said you want it all to stop." This is more effective than pretending everything is normal.
If you are worried about suicide or self-harm, ask directly. You can say, "Are you thinking about hurting yourself?" or "Are you thinking about suicide?" Clear questions do not create danger. They help you understand whether the risk is serious.
If the answer is yes, or if the person gives an unclear answer that still worries you, involve a trusted adult immediately. Tell the person, "I care about you too much to keep this secret." This is one of the most important rules in mental health safety: do not promise to keep suicidal thoughts secret.
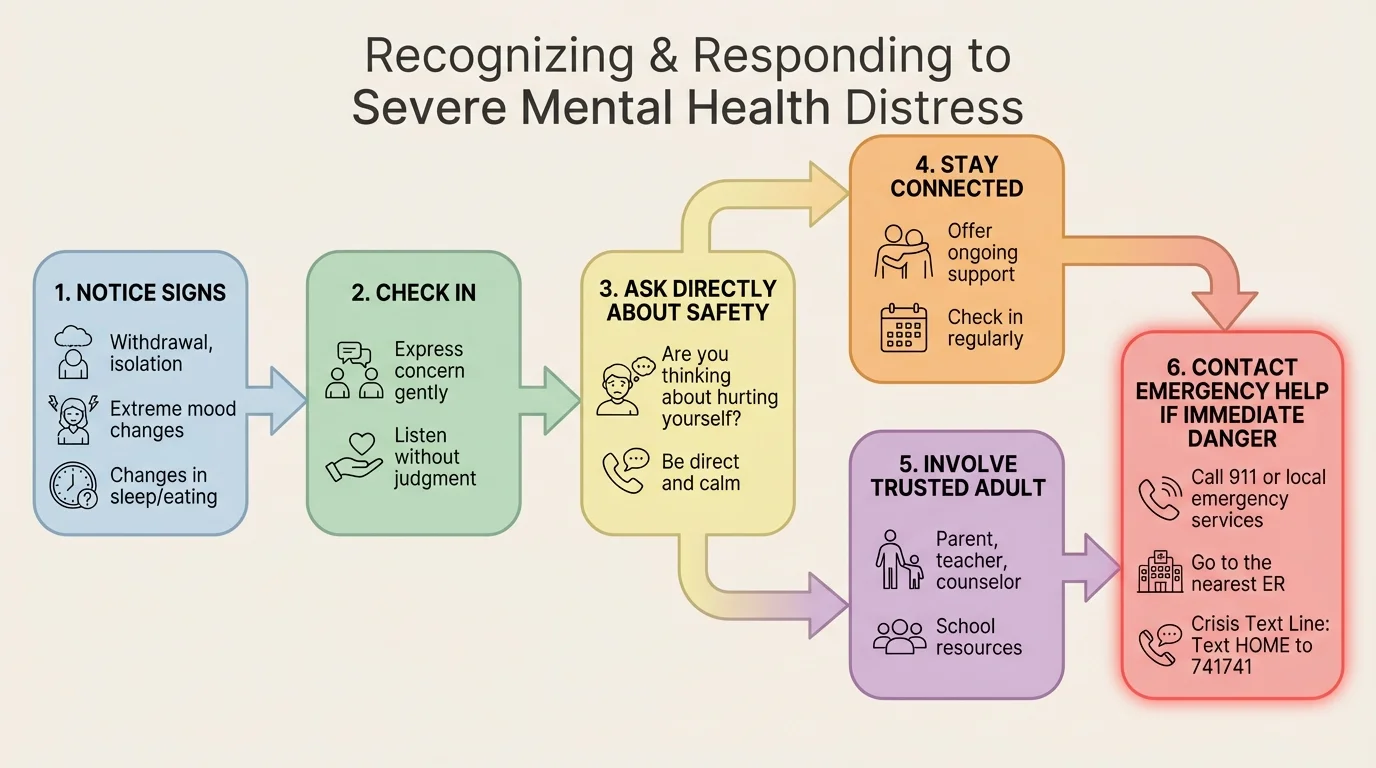
If the danger seems immediate, stay connected while help is being contacted. That may mean keeping them on a call, staying in a chat, contacting a nearby adult who can physically reach them, calling a crisis line with them, or calling emergency services if necessary. As with the urgency levels in [Figure 2], the more immediate the risk, the faster you act.
If they say they are not in immediate danger but still seem overwhelmed, encourage professional help and still tell a trusted adult when the warning signs are serious. You are not betraying them. You are protecting them.
Supportive conversation with a peer
Step 1: Name what you noticed
"You've stopped replying and your messages sound really down. I'm worried about you."
Step 2: Ask directly
"Are you thinking about hurting yourself or ending your life?"
Step 3: Respond without judgment
"Thank you for telling me. I'm staying with you while we get help."
Step 4: Involve an adult
"I'm contacting your parent, guardian, or another trusted adult now because your safety matters."
The goal is care plus action, not care without action.
What should you avoid? Do not argue, dare them to stay alive, make everything about yourself, send guilt-heavy messages, or promise secrecy. Do not say "You're just being dramatic," "Other people have it worse," or "You don't mean that." Those responses can increase shame and isolation.
When emotions are intense, people often freeze because they do not know what to say. A simple script is enough.
For yourself: "I need help with my mental health today." "I'm having thoughts of hurting myself." "I do not feel safe being alone." "Please stay with me while we get support."
For a peer: "I'm really glad you told me." "You matter to me." "I'm going to help you connect with an adult right now." "Are you safe at this moment?" "Can you move to where another adult is?"
"Take it seriously, stay calm, and get help."
— A strong rule for mental health crises
Notice what these scripts have in common: they are short, direct, and focused on safety. In a crisis, clear beats perfect.
Many people delay help because of shame, fear, or uncertainty. They worry about being a burden, getting in trouble, losing privacy, or being seen differently. Some think they need to be "bad enough" to deserve support. That belief is dangerous. You do not need to wait until things become extreme.
Another barrier is the idea that you should handle it on your own. Stigma can make people hide pain because they fear judgment. But mental health crises are health issues, not character flaws. Getting help early often prevents more serious harm later.
You might also worry about overreacting for a friend. If a person is upset that you involved an adult, that does not automatically mean you were wrong. When safety is on the line, protecting life matters more than protecting comfort.
You do not need certainty before seeking help. You need enough concern to act responsibly. If the signs point to danger, involve support.
Privacy matters, but secrecy is different. Privacy means sharing information carefully with the right people. Secrecy means hiding dangerous information when someone may be at risk. Choose privacy, not secrecy.
Recognizing severe distress matters most in crisis, but everyday habits can make help-seeking easier and can lower risk over time. These habits do not replace professional care, but they support resilience, which is your ability to recover, adapt, and keep using healthy supports during hard times.
Protective habits include keeping a regular sleep routine, eating consistently, limiting substance use, staying connected with at least one supportive person, noticing your stress level early, taking breaks from harmful online content, and having a list of people you can contact. You do not need a perfect routine. You need a realistic one.
Try This: Make a personal warning-sign list with three columns: "What I notice," "What helps a little," and "Who I contact." For example, "stop replying," "sleep all day," and "thoughts get dark" can go in the first column. In the second, write actions such as "sit near family," "put phone on speaker and call someone," or "go outside for five minutes." In the third, write actual names.
It also helps to know your early signs before you reach crisis. If you understand your own patterns, you can get support sooner. That is a major part of self-management: noticing what is happening, responding in healthy ways, and asking for help before the situation becomes dangerous.
There are moments when the only correct priority is immediate safety. If you or someone else has a suicide plan, access to means, has taken steps toward an attempt, has already attempted, or cannot agree to stay safe, contact emergency services or a crisis line immediately and alert a trusted adult right away. Do not leave the person alone if you can safely stay connected.
If location is a problem because the person is online, ask where they are and who is nearby. If needed, contact a parent, guardian, another trusted adult, emergency services, or platform safety reporting tools while staying in contact. A digital conversation can still be a real emergency.
After a crisis, follow-up matters. Keep encouraging treatment, check-ins, and support from adults and professionals. Severe distress is not always solved by one conversation. But one conversation can begin protection, treatment, and hope.