Many dangerous situations do not look dramatic at first. A person says they are "just tired," a friend takes "just one pill," someone mixes medications without checking labels, or a bad headache turns into something much more serious. The difference between a close call and a tragedy is often one decision made in the first few minutes.
As you get older, people expect you to make more choices on your own. You may manage your own medications, go to social events, work a part-time job, stay home without adults nearby, or help someone during a crisis. That means safety is not just about following rules. It is about noticing risk, thinking clearly under pressure, and acting fast enough to protect health and life.
Good safety decisions lower harm. Poor safety decisions can lead to poisoning, overdose, injuries, long-term health problems, legal trouble, or delayed emergency care. Sometimes the most mature choice is not doing something bold. It is stopping, checking, and getting help.
Emergency is a situation where someone's life, breathing, brain function, or major body systems may be in immediate danger and quick action is needed.
Overdose is when a person takes more of a drug or substance than the body can safely handle.
Poisoning happens when a chemical, medication, gas, or other substance harms the body after being swallowed, inhaled, absorbed, or injected.
You do not need medical training to make a smart first decision. You do need a calm process, awareness of common warning signs, and the confidence to ask for help early instead of too late.
Not every dangerous substance is illegal. Risk can come from prescription medications, over-the-counter pain relievers, alcohol, nicotine, e-liquids, cannabis products where legal, supplements, cleaning products, and unknown pills or powders. One of the biggest mistakes people make is assuming something is safe because it is common, sold in a store, or given by someone they know.
A situation involving substance misuse can include taking a medication in the wrong dose, using someone else's prescription, mixing alcohol with medicine, combining stimulants with energy drinks, or using a product without knowing what is in it. Even legal products can become dangerous when mixed, overused, or taken by the wrong person.
Prescription medications deserve special caution. If a bottle says take one tablet every six hours, taking two because the pain feels worse is not a small change. It can turn into an overdose. Some medicines also interact with other drugs, alcohol, or certain foods. Reading the label matters.
Over-the-counter medicines can also be misused. Pain relievers, cough medicines, sleep aids, and cold medications may seem ordinary, but taking too much can damage the liver, affect heart rhythm, raise blood pressure, or slow breathing. Household chemicals are another major risk. Bleach, ammonia, detergents, and automotive fluids are not just "products." They are chemicals that can burn skin, damage lungs, or poison the body.
Some dangerous substance combinations happen with everyday items. For example, mixing certain cleaning products can release toxic gases, and combining alcohol with some prescription medicines can make breathing dangerously slow.
One more rule is simple and powerful: if you cannot clearly identify a pill, liquid, vape cartridge, powder, or edible, treat it as unsafe. Unknown substances are especially risky because appearance tells you almost nothing. Counterfeit pills may look real but contain completely different drugs.
When you face a risky situation, use a quick framework, as shown in [Figure 1]: stop, assess, choose, act, and get help if needed. This keeps you from making impulsive choices just because other people are relaxed, joking, or pressuring you.
Stop. Pause before taking, sharing, smelling, tasting, mixing, or touching a substance. A pause of even a few seconds can prevent a bad decision.
Assess. Ask: What is it? Where did it come from? Is it labeled? Who is offering it? Is it prescribed to me? Could it interact with something already taken today? Is the person having symptoms? Is there a safer option?
Choose. If the source is unclear, the label is missing, the dose is uncertain, or mixing is involved, the safest choice is usually do not use it. If symptoms are severe, choose emergency help over waiting.
Act. Move away from danger, call for help, follow the medication label, contact Poison Control if poisoning is possible, or call emergency services if the person is in immediate danger.
Get help. A trusted adult, pharmacist, nurse line, Poison Control, or emergency operator can help you make the next right move. Asking for help is a safety skill, not weakness.
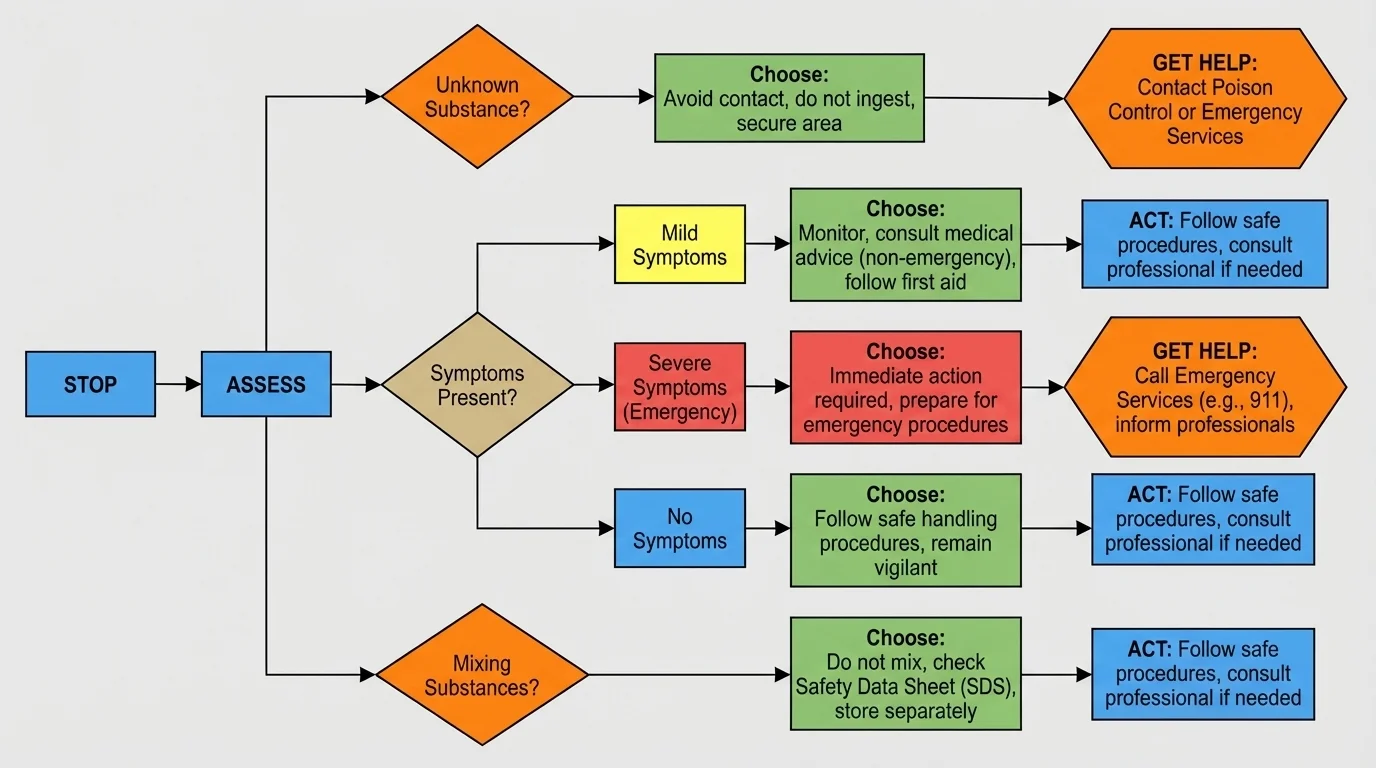
This framework applies to more than drugs or chemicals. It also helps with a suspicious online challenge, an unsafe dare at a social event, taking extra supplements for sports performance, or using a friend's medication before work or a long drive. The same logic applies: identify the risk, avoid guessing, and choose the safer path.
Why mixing is especially risky
Many serious emergencies happen because two or more substances are combined. Depressants such as alcohol and some pain or sleep medicines can slow breathing. Stimulants can raise heart rate and body temperature. A person may think each amount is "small," but the combined effect can be dangerous. You cannot rely on how someone "usually feels" after taking something, because the body's response can change with dose, body size, hydration, fatigue, illness, and what else was taken.
A smart safety decision is often based on incomplete information. You usually do not get perfect certainty. You make the best choice from warning signs, labels, behavior, symptoms, and the possible cost of being wrong. When the possible cost is severe injury or death, it makes sense to act early.
Some patterns should immediately raise concern, as [Figure 2] shows. You do not need to diagnose the exact problem. You only need to recognize that the situation may be an emergency.
Substance-related red flags include a person who is hard to wake up, breathing very slowly, turning blue or gray around the lips, vomiting while unconscious, acting extremely confused, seizing, collapsing, or becoming suddenly violent or severely agitated. These can point to overdose, poisoning, or another urgent medical issue.
Medical emergencies are not limited to substances. Trouble breathing, severe allergic reaction, chest pain, one-sided weakness, sudden face drooping, slurred speech, heavy bleeding that will not stop, fainting, severe burns, signs of heat stroke, and thoughts or statements about self-harm all require serious attention.
A allergic reaction may start with hives or swelling, but if the throat feels tight, breathing gets hard, or the person becomes dizzy, it can become life-threatening fast. A possible stroke often shows up as sudden face drooping, arm weakness, or speech difficulty. In stroke care, time matters because brain cells are at risk the longer blood flow is blocked.
| Warning sign | Why it matters | Safer response |
|---|---|---|
| Slow or stopped breathing | Oxygen may not be reaching the brain | Call emergency services immediately |
| Unconscious and not responding | Can signal overdose, head injury, or medical crisis | Call emergency services and monitor breathing |
| Blue lips or gray skin tone | Possible severe lack of oxygen | Treat as an emergency |
| Severe bleeding | Rapid blood loss can become life-threatening | Apply firm pressure and call for help |
| Face droop, arm weakness, slurred speech | Possible stroke | Call emergency services immediately |
| Chest pain with shortness of breath | Possible heart or lung emergency | Call emergency services |
| Threats of self-harm or suicide | Immediate mental health danger | Stay with the person and get emergency help |
Table 1. Common emergency warning signs, why they are serious, and the safest immediate response.
Notice the pattern: if breathing, consciousness, heavy bleeding, brain function, or severe pain is involved, do not wait for things to "probably pass." Delayed action is one of the most dangerous choices people make.

When a situation turns serious, as shown in [Figure 3], your goals are clear: protect yourself, get help, support the person, and avoid making the situation worse. The order matters. If there is fire, toxic fumes, violence, traffic, or exposed electricity, move to safety first if you can do so without increasing danger.
If someone may be having an overdose, poisoning, or major medical emergency, call emergency services right away. Give your exact location, what happened, the person's age if known, whether they are awake, and whether they are breathing. If you are nervous, focus on the basics. Operators are trained to guide you.
If poisoning may be involved and the person is awake and stable, Poison Control can be important. Do not force vomiting unless a medical professional specifically tells you to. Vomiting can make some poisonings worse.
If the person is unconscious but breathing, place them on their side if possible. This recovery position helps keep the airway clearer and lowers the chance of choking if they vomit.
If the person is not breathing normally, that is an emergency. Call immediately and follow dispatcher instructions. In some communities, bystanders may also use naloxone if opioid overdose is suspected. Naloxone can temporarily reverse the effects of certain opioid overdoses, but emergency care is still needed because the danger can return.
Do not give food, drinks, extra medicine, or random home remedies to a person who is severely impaired, choking, or barely awake. Do not leave them alone because you feel uncomfortable or worried about getting in trouble. Staying and getting help can save a life.
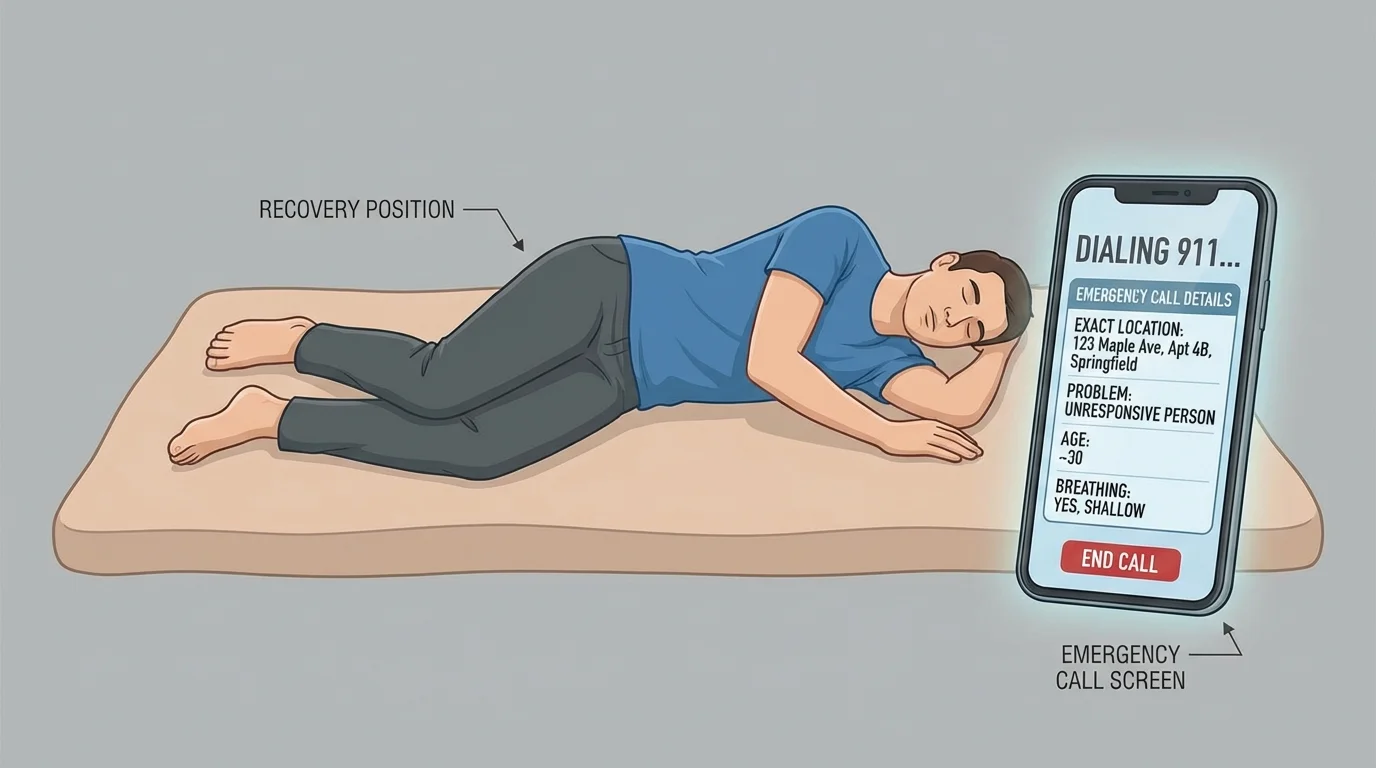
Case study: A friend becomes unresponsive after a social event
Step 1: Notice the red flags
Your friend is very difficult to wake, speech is unclear, and breathing seems slow.
Step 2: Choose safety over embarrassment
Do not assume they just need sleep. Slow breathing and unresponsiveness are emergency signs.
Step 3: Call and report clearly
Call emergency services, give the address, describe the breathing and level of responsiveness, and mention any known alcohol or drug use.
Step 4: Support while waiting
Keep the airway clear, place them on their side if breathing, and stay nearby to monitor changes.
The safest choice is fast action. Waiting because you fear drama or punishment can cost critical time.
Later, when you review what happened, the same response pattern still makes sense. As we saw in [Figure 3], protecting the airway and giving clear information to emergency responders are practical actions that bystanders can take even without advanced medical training.
[Figure 4] shows how social situations can combine several risks at once: unfamiliar substances, pressure to fit in, transportation problems, and people assuming someone else will handle the situation. This is why you need decisions made in advance, not only in the moment.
Protect your drink and food. Do not leave them unattended and then keep consuming them. Do not take pills, gummies, vapes, or powders from someone just because they seem relaxed about it. "Everyone does it" is not evidence of safety. It is social pressure.
Transportation is part of substance safety. If a driver has been drinking or using drugs, or seems unusually tired or reckless, do not get in the vehicle. Call someone, use a rideshare carefully, or make another plan. Verify the car and driver information before getting in.
If a friend wants to do something unsafe, you do not need a perfect speech. Short responses work: "No, I don't know what that is." "I'm not mixing stuff." "I'm leaving." "You need help right now." Clear words are safer than vague ones.
You also need to avoid becoming a second victim. If someone is exposed to fumes in a closed garage, for example, rushing in without thinking can put you in danger too. Call for help and protect yourself first. If there is violence or a weapon present, get to safety and contact emergency services rather than trying to physically control the situation.

Supportive friendships include safety. A real friend does not push you to ignore labels, hide symptoms, or "sleep it off" when a person may be in danger. Good friends respect boundaries, help each other leave unsafe situations, and act when something feels wrong.
"If you are not sure whether it is serious, treat it like it might be."
That principle is not about panic. It is about understanding the cost of delay. Calling for help and finding out the person is okay is far better than staying quiet while a condition gets worse.
Not every harmful decision causes an immediate emergency. Some choices slowly increase risk over weeks, months, or years. Repeated vaping, heavy drinking, misuse of prescription medications, using stimulants to stay awake, and repeated energy drink overuse can affect the heart, lungs, brain, sleep, mood, and decision-making.
Tolerance means the body becomes less responsive to a substance over time, so a person needs more to get the same effect. Dependence means the body or mind begins to rely on that substance to function or feel normal. These patterns increase the chance of addiction, risky behavior, and overdose.
Mental health is part of serious health risk too. If someone talks about feeling hopeless, says people would be better off without them, gives away important possessions, or talks about self-harm, take it seriously. Stay with them if it is safe, contact a trusted adult or emergency service, and do not keep suicidal intent secret.
Health emergencies are not always visible from the outside. A person can be in serious danger from internal bleeding, severe dehydration, alcohol poisoning, or suicidal crisis even if there is no dramatic injury.
Another slow-building danger is delayed care. Some people ignore symptoms because they do not want attention, cost, or conflict. But chest pain, worsening shortness of breath, severe abdominal pain, repeated fainting, or rapidly spreading rash are not problems to "wait out" without guidance. Early treatment often prevents bigger emergencies later.
The pattern from [Figure 2] still applies here: when core body functions or major warning signs are involved, the safest decision is to escalate your response instead of minimizing the problem.
Strong safety decisions are easier when you prepare before anything goes wrong. Keep medicines in original containers. Follow dose directions exactly. Do not share prescriptions. Store medications, alcohol, nicotine products, and chemicals out of reach of children and away from pets. Read labels before use, especially for cleaning products and pain relievers.
Create a basic emergency setup on your phone. Save emergency contacts, your home address, and local emergency numbers. If you have allergies, asthma, diabetes, seizures, or another medical condition, make sure trusted people know what to do in a crisis. If you carry an inhaler, epinephrine auto-injector, or other important medication, know where it is at all times.
Think through likely scenarios. If you are home alone and there is a fire alarm, where do you go? If a relative becomes unresponsive, who do you call? If you feel unsafe during an online-arranged meetup in the community, how do you leave and who is your backup contact? A plan makes panic less likely.
Try this today: build a personal safety checklist
Step 1: Program contacts
Add emergency contacts, Poison Control, and at least one trusted adult to your phone favorites.
Step 2: Check labels
Look at one medication and one household chemical in your home. Read the directions and warnings.
Step 3: Identify risks
Notice any unlabeled pills, open vape products, or chemicals stored unsafely, and tell a responsible adult if needed.
Step 4: Make an exit plan
Decide how you would leave a social situation if the people, substances, or transportation became unsafe.
These are small actions, but they make safer decisions much easier under pressure.
Preparation also includes communication. If you need help, be direct. Say what is happening, where you are, and what you need. For example: "My friend is not waking up and breathing slowly. We are at 214 Pine Street." Clear communication speeds up good help.
Good judgment is not about knowing every medical fact. It is about recognizing uncertainty, respecting warning signs, and understanding that your choices affect real bodies and real lives. It means not taking unknown substances, not mixing products casually, not leaving an impaired person alone, and not treating severe symptoms like a small inconvenience.
The safest decision is often the one that feels less convenient in the moment: reading the label, calling for help, saying no, leaving early, or interrupting the group's plans because someone is in danger. That is not overreacting. That is maturity.