One of the most dangerous myths about harmful situations is that you must be able to handle them alone. In real life, people are often pressured when they are tired, scared, confused, embarrassed, or worried about being judged. That is exactly why support systems matter. A good support system does not just comfort you. It helps you think clearly, make safer choices, get medical care, leave risky situations, and protect your rights.
Support systems can include trusted adults, relatives, older siblings, mentors, medical professionals, hotlines, community organizations, and emergency services. They can also include practical tools such as saved phone numbers, shared locations, screenshots, ride options, and a plan for what to say when you need help fast. The goal is not to know everything. The goal is to know who to contact, when, and why.
If someone is pressuring you into sexual activity, controlling who you talk to, threatening to share private messages, ignoring your boundaries, or making you feel unsafe, the problem is bigger than a "relationship issue." If you have symptoms of illness, think you might have an STI, are worried about pregnancy, are having panic attacks, or feel like you might harm yourself, the problem is bigger than "just stress." In both cases, waiting too long can make things worse.
Strong support systems help in at least four ways. First, they provide safety. Second, they provide perspective when pressure is making you doubt yourself. Third, they provide resources, such as transportation, medical care, reporting options, or crisis counseling. Fourth, they create accountability, which matters when another person is trying to isolate or manipulate you.
Coercion is pressure, manipulation, threats, guilt, or intimidation used to push someone into doing something they do not freely choose.
Unsafe relationship refers to a relationship in which someone ignores boundaries, controls, threatens, humiliates, isolates, or harms another person emotionally, physically, sexually, or digitally.
Support system is the group of people, services, and tools you can rely on for safety, guidance, care, and practical help.
It is also important to understand that needing help is not a sign of weakness. It is a sign that you are responding to risk in a smart way. People who get support early often have more options than people who stay silent.
Before you can choose the right support, you need to name what is happening. That can be hard because harmful behavior is not always dramatic. Sometimes it looks like repeated guilt trips: "If you loved me, you would." Sometimes it looks like monitoring: demanding passwords, checking your location constantly, or getting angry when you do not reply immediately. Sometimes it looks like health neglect: ignoring symptoms because you are nervous to tell anyone.
Common signs of coercive pressure include repeated begging after you said no, threats to break up, threats to embarrass you online, pressure involving alcohol or drugs, and statements that make you responsible for the other person's feelings or actions. Consent is not real if you are scared, cornered, manipulated, or worn down. Consent must be freely given.
Common signs of an unsafe relationship include jealousy framed as love, constant criticism, isolating you from friends or family, controlling your clothes or activities, invading your privacy, threatening self-harm to control you, and making you feel afraid to disagree. In online relationships, this can include demands for explicit photos, pressure during video chats, blackmail, or nonstop tracking through apps and accounts.
Health concerns can also require support even when no relationship issue is involved. You may need help if you have symptoms like severe pain, fever, unusual discharge, fainting, trouble breathing, possible exposure to an STI, signs of depression, panic, or thoughts of self-harm. Some health concerns are urgent; others still matter even if they are not emergencies.
Many people delay asking for help because they think their situation is "not bad enough." In reality, support works best when you reach out early, before pressure or symptoms become more severe.
A useful question is: "Do I feel more free, more safe, and more respected in this situation — or less?" If the answer is less, that is a signal to involve support.
[Figure 1] Different problems need different helpers. A clear way to think about support is in layers. The people closest to you may give immediate comfort and practical help, while professionals and emergency services handle specialized or urgent needs.
Your first layer is your personal network: a parent, guardian, aunt, uncle, older cousin, trusted family friend, coach, youth leader, employer, mentor, or friend who is steady and respectful. This layer is often the fastest to contact. They may pick you up, stay on the phone with you, help you leave a situation, or sit with you while you make another call.
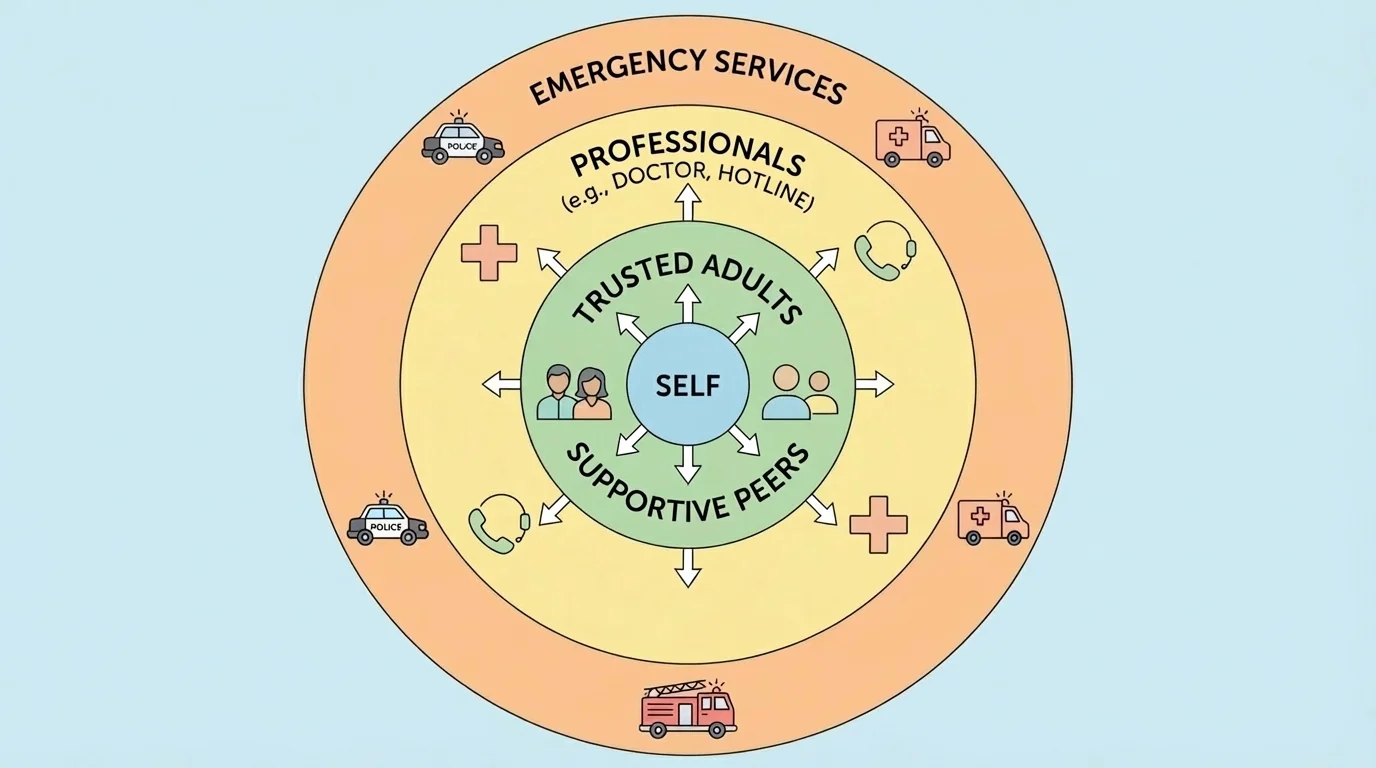
Your second layer is professional support. This includes doctors, nurses, sexual health clinics, therapists, crisis counselors, domestic violence advocates, sexual assault hotlines, and mental health hotlines. These people have training, confidentiality rules in many situations, and knowledge about medical care, documentation, and safety planning.
Your third layer is formal authority. This includes emergency services, law enforcement, and emergency medical care. Not every situation belongs here, but immediate danger does. If someone is threatening you, physically harming you, refusing to let you leave, or you are having a medical emergency, waiting for a casual conversation is not the right move.
Your fourth layer is digital support tools. These are not replacements for people, but they help. Useful tools include emergency contacts in your phone, a shared location with a trusted adult, ride apps, screenshot folders, blocked lists, privacy settings, and a code word that tells someone you need help without explaining everything.
As you saw in [Figure 1], support systems work best when they are not just one person. If one person does not answer, you still need options.
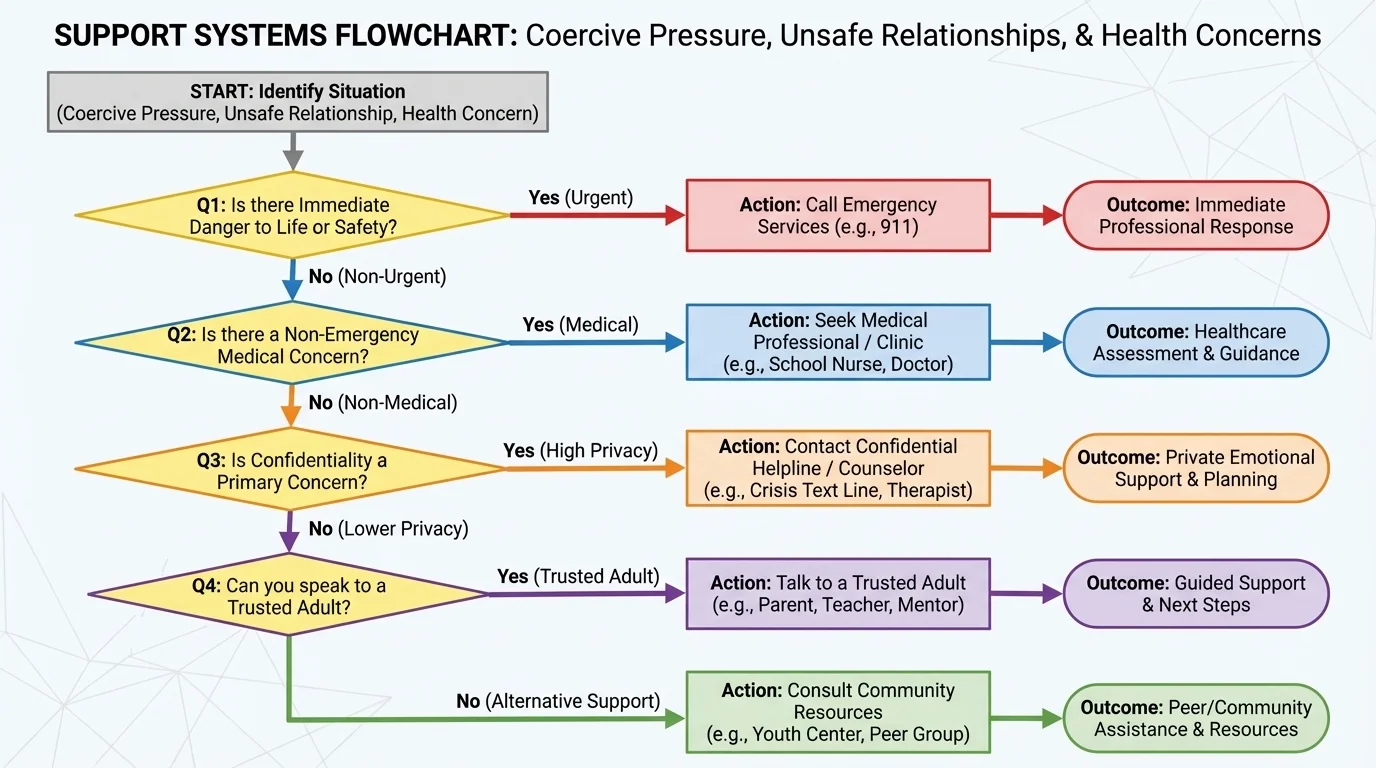
When you are stressed, it helps to sort support options by four questions, and [Figure 2] lays out that decision process visually: How urgent is this? Do I need privacy? Do I need expert advice? Am I in immediate danger? The answers guide where you start.
A trusted friend may be great for staying on a call with you, helping you not feel alone, or encouraging you to seek more help. But a friend may not know what to do if you need medical care, legal reporting information, or safety planning. A trusted adult often has more power to arrange transportation, protect you, or help you make difficult calls.
A clinic or doctor is the right choice when the issue involves symptoms, sexual health questions, pregnancy concerns, injury, or medical evidence. A hotline is especially useful when you need anonymous advice, emotional support, or guidance on what to do next. Emergency services are for immediate threats to life or safety.
Use the table below to compare common support options.
| Support option | Best for | Strengths | Limits |
|---|---|---|---|
| Trusted friend | Immediate emotional support, staying connected | Fast, familiar, comforting | May lack training or authority |
| Trusted adult | Safety planning, transportation, guidance, intervention | More experience, can take action | Not always available immediately |
| Doctor or clinic | Symptoms, STI testing, pregnancy concerns, injury | Medical expertise, treatment options | May require appointment or travel |
| Hotline or crisis line | Anonymous advice, emotional support, crisis guidance | Available quickly, trained responders | Cannot physically come get you |
| Emergency services | Immediate danger, assault, severe medical emergency | Rapid emergency response | Used for urgent situations only |
Table 1. Comparison of common support options for unsafe relationship and health-related situations.
Notice that "best support" does not always mean "only support." You might text a friend, call a trusted adult, and go to a clinic all in the same situation. Support systems are often strongest when several layers work together.
When people panic, they often try to explain everything perfectly. You do not need a perfect speech. A simple plan makes it easier to act even when you feel overwhelmed.
Step 1: Decide if you are in immediate danger. If someone is threatening you, blocking you from leaving, driving recklessly, becoming violent, or you are having a severe medical emergency, call emergency services right away.
Step 2: Contact one trusted person with a direct message. Try: "I need help right now. Can you call me?" or "I do not feel safe. Can you stay on the phone and help me leave?" If the issue is health-related, try: "I have a health concern and need to get checked today. Can you help me get care?"
Step 3: Share practical details. Tell them where you are, who is with you, whether you need a ride, whether you want them to stay on the phone, and whether you need medical help. If texting is safer than calling, text. If talking is not safe, use a code word you planned in advance.
Step 4: Preserve important information. Save screenshots, messages, call logs, dates, and photos of injuries if relevant. Documentation can help medical professionals, advocates, or authorities understand the situation. Do not risk your safety just to collect evidence, though. Safety comes first.
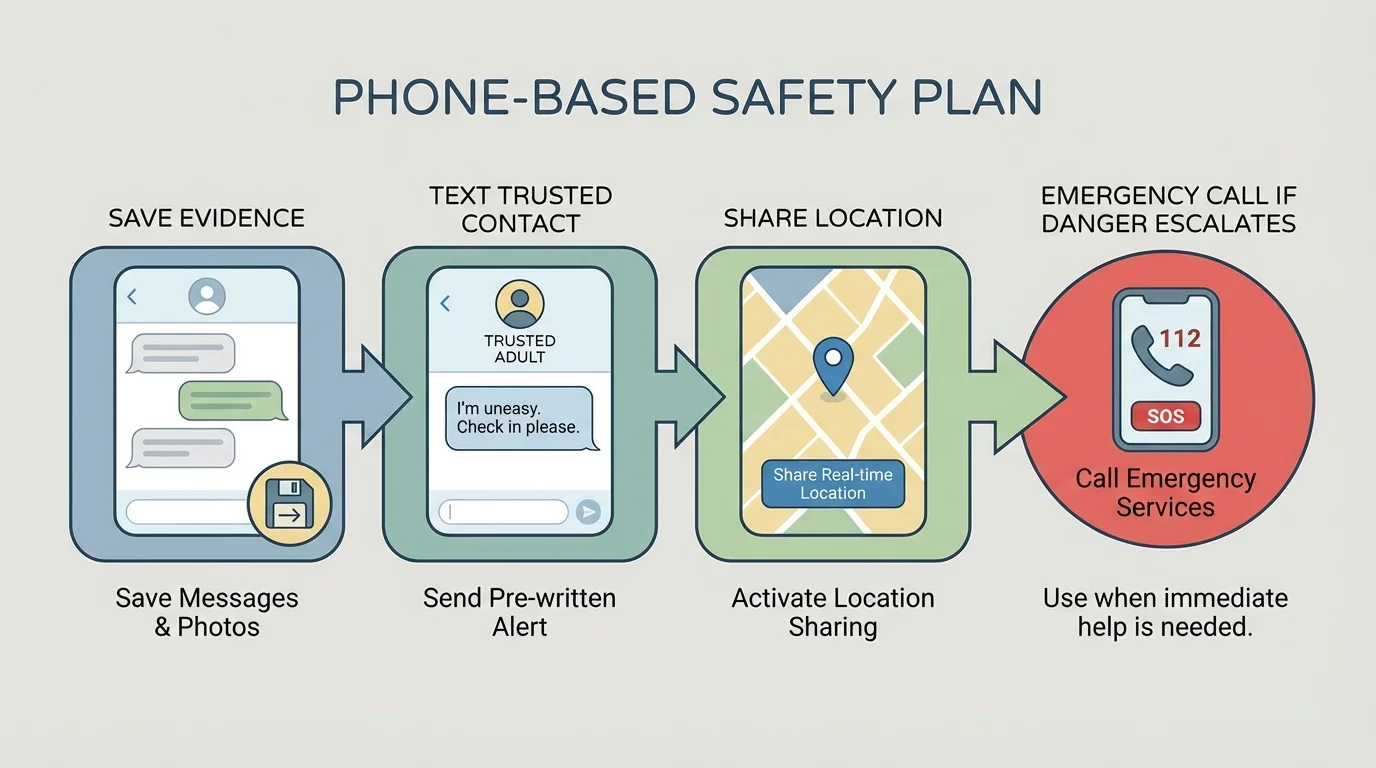
Step 5: Move toward safety. Go to a public place, leave the chat, log out of shared accounts, block a person if needed, or get to an adult who can stay with you. If you are meeting someone in person and they start pressuring you, you are allowed to leave without explaining more.
Step 6: Follow through with the next support layer. That might mean scheduling a clinic visit, calling a hotline, asking for a ride, changing passwords, or making a report.
Example: A clear help text
Step 1: State the problem simply.
"I do not feel safe with the person I'm with."
Step 2: State what you need.
"Can you call me now and help me leave?"
Step 3: Add location or urgency.
"I'm at the coffee shop on Pine Street. Please stay on the phone."
This works because it is short, specific, and actionable.
If you are worried that someone will see your messages, use shorter wording, delete messages only if that improves safety, and switch to a safer device when possible. In some situations, calling from a different phone may be safer than using your own.
Sexual pressure requires immediate clarity. If someone keeps pushing after you say no, that is not romance, and it is not your job to manage their disappointment. Reach out to a trusted adult, hotline, or advocate if you feel trapped, pressured, threatened, or confused about what happened. If any sexual contact was not fully consensual, medical care can matter even if there are no visible injuries.
If you are worried about pregnancy or an STI, choose medical support early. A confidentiality question is common here: you may want private care or private advice before talking with others. A clinic, doctor, or hotline can explain testing, treatment, and next steps. Delaying care out of embarrassment can create bigger health problems.
If a partner or online contact is controlling, threatening, blackmailing, or monitoring you, broaden your support network. Tell a trusted adult. Save evidence if safe. Change passwords from a secure device. Review app permissions and location sharing. As the phone sequence in [Figure 3] illustrates, digital safety is part of personal safety.
Mental health concerns also deserve real support. If you feel hopeless, panicked, unable to function, or you are thinking about hurting yourself, contact a crisis line, trusted adult, or emergency service depending on urgency. You do not need to wait until things become extreme to ask for help.
"You are allowed to protect your peace, your health, and your safety without first convincing someone else that the problem is serious enough."
If another person says you are overreacting, that does not erase the warning signs. As [Figure 3] suggests, your feelings are not the only evidence, but they are important data. Fear, dread, confusion, and pressure are signals worth taking seriously.
The best time to build a support system is before a crisis. Start by listing at least three people you could contact: one family-based adult, one non-family adult, and one peer who is reliable under stress. Add a clinic number, a crisis line, and emergency contacts to your phone.
Create a mini safety plan. Decide on a code word. Keep your phone charged. Know how you would leave an unsafe location. Think about transportation. Review your privacy settings. If you ever share your location with someone, make sure it is your choice and that you know how to turn it off.
Prepared support is stronger than last-minute support. When people plan ahead, they do not have to invent a response in the middle of fear or pressure. Even small steps—saving numbers, identifying one trusted adult, deciding on a code word—make it easier to act quickly and safely.
Also think about the quality of your support. A good support person listens, respects your choices, takes concerns seriously, and helps you move toward safety and care. A poor support person minimizes, blames, gossips, or pressures you into decisions you are not ready to make. Part of analyzing support systems is judging not just who is available, but who is actually safe and helpful.
Scenario one: You are on a date, and the other person keeps insisting on going somewhere private after you already said no. The best support sequence is to contact a trusted adult or friend immediately, leave the situation, and stay connected by phone until you are safe. If the person will not let you leave, it becomes an emergency.
Scenario two: Someone you are talking to online threatens to share private photos unless you send more. This is abuse, not drama. Stop negotiating. Save evidence if safe, tell a trusted adult, block the person, secure accounts, and contact a hotline or authorities if needed. As the decision path in [Figure 2] shows, blackmail and safety risk move the problem beyond simple peer advice.
Scenario three: You are worried you may have been exposed to an STI, but you feel embarrassed. The best support may start with a clinic, doctor, or hotline rather than a friend. A trusted adult can help with transportation or appointment support. The right support is the one that gets you accurate care quickly.
Scenario four: A partner constantly demands your passwords and gets angry if you take too long to reply. That is controlling behavior. Personal support plus digital safety steps are important here. Tell a trusted adult, change passwords, turn off unwanted location sharing, and assess whether the relationship is safe to continue.
Scenario five: You feel overwhelmed, cannot stop crying, and are having thoughts of self-harm late at night. In that moment, do not wait for morning if the risk feels immediate. Contact a crisis line, wake a trusted adult, or call emergency services if needed. Safety takes priority over embarrassment.
Real maturity is not pretending nothing affects you. It is knowing how to recognize risk, choose support, and take action. The people who stay safest are not always the strongest or most confident-looking. Often, they are the ones who know when to reach out.