Many health problems become stressful not because they are severe, but because people have no plan. They become stressful because people have no plan. A sore throat turns into panic because no one knows what medication is safe, who to call, where an insurance card is, or what symptoms mean "wait and rest" versus "get help now." A personal health plan solves that problem before it starts.
Your health plan is not just for emergencies. It is a practical guide for everyday life. It helps you lower your chances of getting sick or injured, take care of yourself when something minor happens, and know how to get help when a problem is bigger than self-care. That combination matters because being independent is not the same as handling everything alone. Real strength includes knowing when to ask for support.
When you have a plan, you make better decisions under pressure. You waste less time, feel less panic, and are more likely to get the right help. Without a plan, people often do one of two things: they ignore symptoms too long, or they panic and make rushed choices. Neither one is safe.
Think about two different situations. In one, a student starts feeling dizzy, realizes they barely drank water, checks their plan, drinks fluids, eats something balanced, rests, and tells a parent or guardian if the feeling continues. In another, the same student ignores the dizziness all day, keeps scrolling late into the night, skips meals, and finally asks for help only when the problem feels worse. The second situation is more chaotic, more stressful, and sometimes more dangerous.
Personal health plan means a written, usable plan for how you protect your health, respond to common health issues, and get help when needed.
Prevention means actions you take to reduce the chance of illness, injury, or long-term health problems.
Care means the safe steps you take to manage everyday health needs and minor problems.
Help-seeking means knowing when, how, and from whom to get support for physical, mental, or emotional health concerns.
A good plan is personal. It should match your body, your routines, your family situation, your access to transportation, your insurance or clinic options, and the adults you trust. Someone with asthma, for example, needs a different plan from someone with food allergies. Someone who plays sports in hot weather may need more focus on hydration and injury prevention. Someone dealing with anxiety may need clear mental health support steps built into the plan.
A strong health plan has three connected parts, as [Figure 1] shows: prevention, care, and help-seeking. These are not separate worlds. They work together. Prevention lowers risk. Care helps with small or routine problems. Help-seeking protects you when a problem is too serious, too confusing, or too persistent to handle alone.
Prevention includes habits like getting enough sleep, staying current on recommended vaccines, washing your hands, wearing a seat belt, using sunscreen, protecting your hearing, managing stress, and making thoughtful choices about substances and relationships. Care includes things like resting when you are sick, drinking water, reading medicine labels carefully, using basic first-aid supplies correctly, and tracking symptoms. Help-seeking includes contacting a parent, guardian, doctor, counselor, nurse advice line, therapist, urgent care, or emergency services when appropriate.
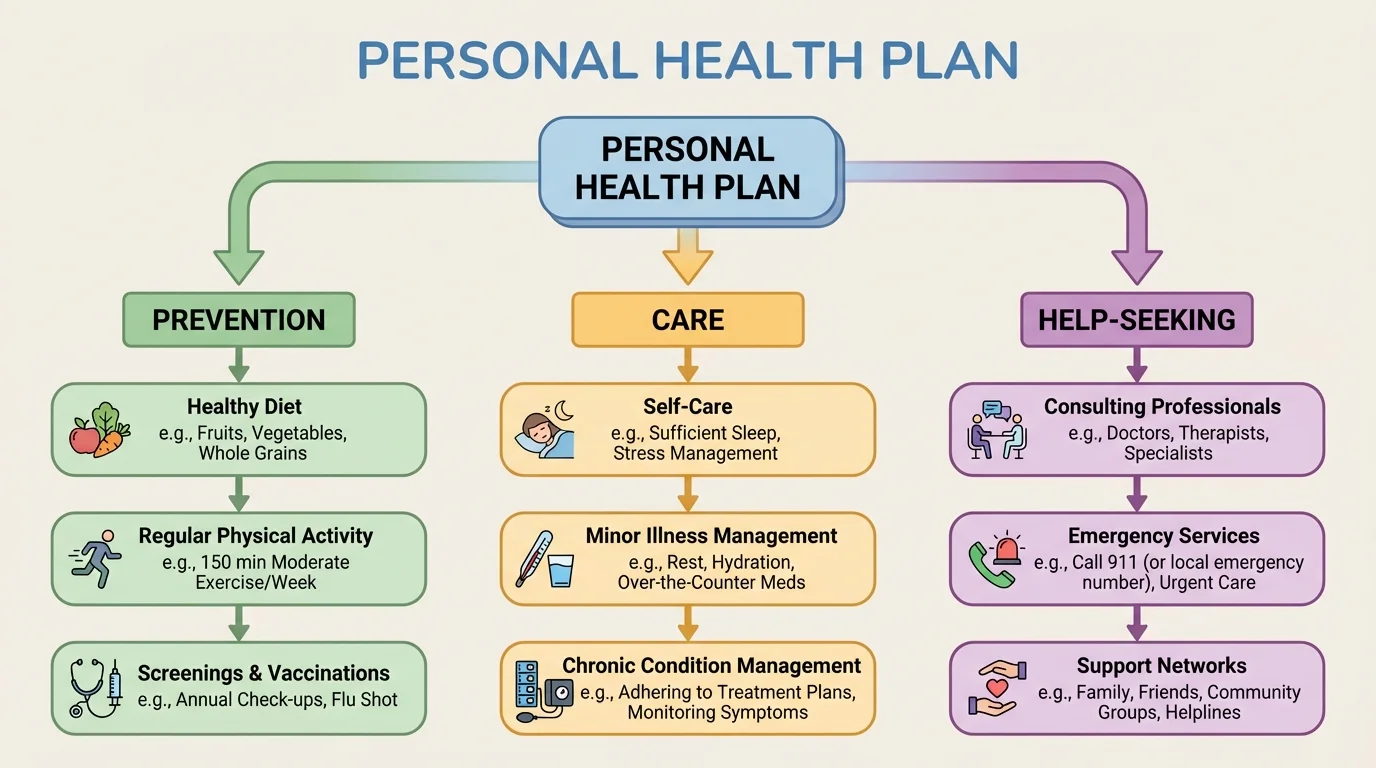
If one part is missing, your plan gets weaker. A person who focuses only on prevention may feel lost once they actually get sick. A person who only knows self-care may wait too long to get help. A person who only seeks help in emergencies may miss the daily habits that prevent bigger problems in the first place.
Before you can build a useful plan, you need to know what "normal" looks like for you. Your usual sleep, energy, mood, stress level, appetite, activity level, and focus all matter. If you normally sleep about 8 hours and suddenly drop to 5 hours for several nights, that is important. If your mood changes noticeably for more than a few days, that matters too. A health plan works better when you can notice changes early.
This is where baseline matters. Your baseline is your typical condition when things are going reasonably well. Knowing it helps you spot warning signs faster. For example, if you usually handle schoolwork calmly but suddenly feel overwhelmed, irritable, and exhausted every day, your plan should tell you what support steps to take instead of assuming you should just "push through."
Your health is a pattern, not a single moment. One late night or one bad meal usually is not a crisis. But repeated patterns can change your energy, mood, focus, immune system, and safety. A personal health plan helps you notice patterns before they become bigger problems.
Start by paying attention to a few basic areas: sleep, food, hydration, movement, stress, mental health, and any known medical needs. You do not need to become obsessed with tracking every detail. You just need enough awareness to recognize when something is off.
It also helps to know your personal risk factors. These might include allergies, asthma, migraines, depression, anxiety, diabetes, a history of injuries, family history of certain conditions, or side effects from a medicine. If you have any diagnosis, regular medication, or known trigger, that belongs in your plan.
Prevention sounds simple, but it is really about systems. If your plan says "sleep more" but you stay up with your phone every night, that is not a system. If your plan says "drink water" but you never carry a water bottle and forget all day, that is not a system either. The best prevention habits are specific and repeatable.
Here are practical prevention areas to include:
Prevention also includes regular health care, even when you feel fine. That may mean checkups, dental care, vision exams, or following a treatment plan for an ongoing condition. Preventive care can catch problems early, which is usually easier, cheaper, and safer than waiting.
Many common health problems get worse not because they are rare or mysterious, but because people delay basic care. Small issues such as dehydration, untreated cavities, infected cuts, and poor sleep can grow into much bigger problems when ignored.
Another prevention area is boundaries. Protecting your health includes saying no to unsafe dares, avoiding substance use, recognizing pressure in dating or sexual situations, and speaking up when something feels wrong. Prevention is not just about germs and injuries. It is also about decision-making.
Try This: Choose one prevention habit that would make the biggest difference for you this week. Make it concrete. "Drink more water" becomes "fill my bottle before noon and again after dinner." "Sleep earlier" becomes "put my phone across the room at 10:30 p.m."
Care is what you do when prevention was not enough or when everyday health needs still show up. This part of your plan should cover common situations such as headaches, colds, stress, minor cuts, muscle soreness, mild stomach upset, menstrual symptoms, or a low-energy day.
A safe care plan usually includes rest, hydration, simple symptom tracking, and knowing your limits. It may also include approved over-the-counter medicine, but only if you know what it is for, how to use it correctly, and whether a parent, guardian, or healthcare professional has said it is safe for you. Never take random pills from someone else, and never mix medicines casually just because they are sold in stores.
A basic home care kit can help: bandages, a thermometer, tissues, soap, a cold pack, a small notebook or notes app for symptoms, and any personal essentials you use regularly. If you take prescription medication, your plan should say when to take it, what to do if you miss a dose, and who to contact with questions.
Example: handling a mild sore throat safely
Step 1: Check your symptoms.
Ask: Do I also have trouble breathing, severe swelling, dehydration, or a very high fever? If yes, this may be more than a minor issue.
Step 2: Use basic care.
Rest, drink fluids, avoid irritating foods if swallowing hurts, and tell a trusted adult what is going on.
Step 3: Track the pattern.
If symptoms are mild and improving, continue care. If they last several days, get worse, or come with warning signs, move to the help-seeking part of your plan.
This approach is calmer and safer than either ignoring the problem or assuming the worst right away.
Self-care has limits. If you are unsure what is happening, if symptoms are unusual for you, or if you have a condition that can complicate a "small" illness, ask for help sooner. For example, vomiting may be minor for one person but riskier for someone with diabetes or someone who cannot keep fluids down.
[Figure 2] One of the most important parts of health planning is knowing the difference between urgent care, routine care, and an emergency. You do not need to diagnose yourself perfectly. You need to notice warning signs and choose the safest next step.
A useful way to think about this is in three levels: manage at home for now, get help soon, and get emergency help now.
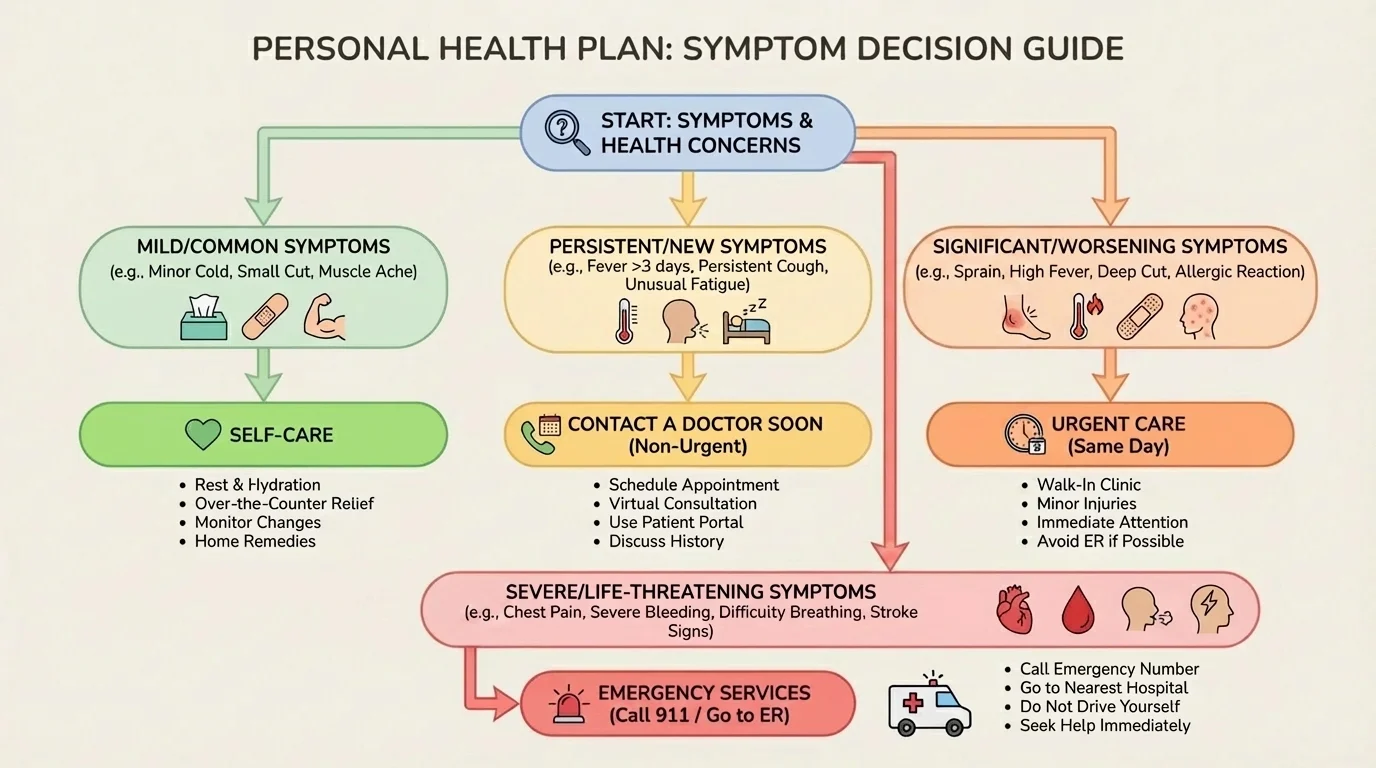
Manage at home for now may fit mild symptoms that are improving with rest, water, food, and time. Examples include a small headache after not drinking enough water, mild muscle soreness after exercise, or a common cold with no severe symptoms.
Get help soon applies when symptoms are not improving, are getting worse, or are affecting daily life. This might include a fever that lasts, repeated vomiting, a painful possible infection, ongoing sadness or anxiety, frequent panic, a rash spreading quickly, worsening pain, or a minor injury that is not healing properly.
Get emergency help now applies to warning signs such as chest pain, trouble breathing, severe allergic reaction, seizure, loss of consciousness, serious head injury, signs of stroke, heavy bleeding that will not stop, suicidal thoughts with immediate danger, or any situation where someone is not safe waiting for a regular appointment.
When in doubt, involve a trusted adult immediately. Waiting too long can turn a manageable problem into a dangerous one. As we saw in [Figure 2], the decision is not about being tough. It is about matching the response to the risk.
| Situation | Likely First Step | What to Watch For |
|---|---|---|
| Mild headache after little water or food | Hydrate, eat, rest | If severe, repeated, or paired with confusion, seek help |
| Small cut | Clean it and bandage it | If bleeding will not stop or signs of infection appear, get help |
| Stress or sadness lasting a day | Rest, coping tools, talk to someone | If it lasts, worsens, or includes hopelessness, seek support soon |
| Trouble breathing | Emergency help | Do not wait to see if it passes |
| Allergic reaction with swelling or wheezing | Emergency help | Use prescribed emergency medication if available |
Table 1. Examples of first responses and warning signs for common health situations.
Help-seeking is a skill. Some people avoid it because they do not want to seem dramatic. Others freeze because they do not know what to say. A plan fixes both problems by giving you words ahead of time.
Use a simple structure: what is happening, how long it has been happening, what you already tried, and what you need now. For example: "I have had a strong headache since this morning. I drank water and ate lunch, but it is getting worse. I need help deciding whether I should rest, call a doctor, or do something else." That is clear, calm, and useful.
Example messages you can actually send
To a parent or guardian:
"I have been feeling dizzy for about an hour. I drank water, but it is not going away. Can you call me or check in?"
To request a medical appointment:
"Hi, I need to schedule an appointment. I have had a sore throat and fever for two days, and symptoms are getting worse."
To ask for mental health support:
"I have been feeling overwhelmed and down for the last two weeks, and it is affecting sleep and schoolwork. I want help talking to a counselor or therapist."
This matters for mental health too. If you feel constantly anxious, unusually numb, hopeless, unable to cope, or unsafe with your own thoughts, that belongs in your health plan just as much as asthma or a broken bone would. Mental health is health.
You should also know who belongs on your support list. This may include a parent, guardian, older sibling, relative, doctor, therapist, clinic, community mentor, coach, or another trusted adult. If one person does not respond, your plan should include a backup contact.
"Asking for help is a strategy, not a weakness."
Privacy matters, but safety matters more. If you are in immediate danger, or someone else is, get help even if it feels uncomfortable. If you are worried about confidentiality, ask directly: "Will this stay private?" A healthcare professional can explain limits, especially when safety is at risk.
[Figure 3] A written plan works better than a plan that only lives in your head. Keep your plan somewhere easy to reach, such as your phone notes, a printed page at home, or both.
Your plan should include: full name, birth date, allergies, medications, health conditions, emergency contacts, doctor or clinic information, insurance information if available, trusted adults, mental health support contacts, prevention habits, common symptoms to watch for, safe home-care steps, and clear signs that mean "get help now."
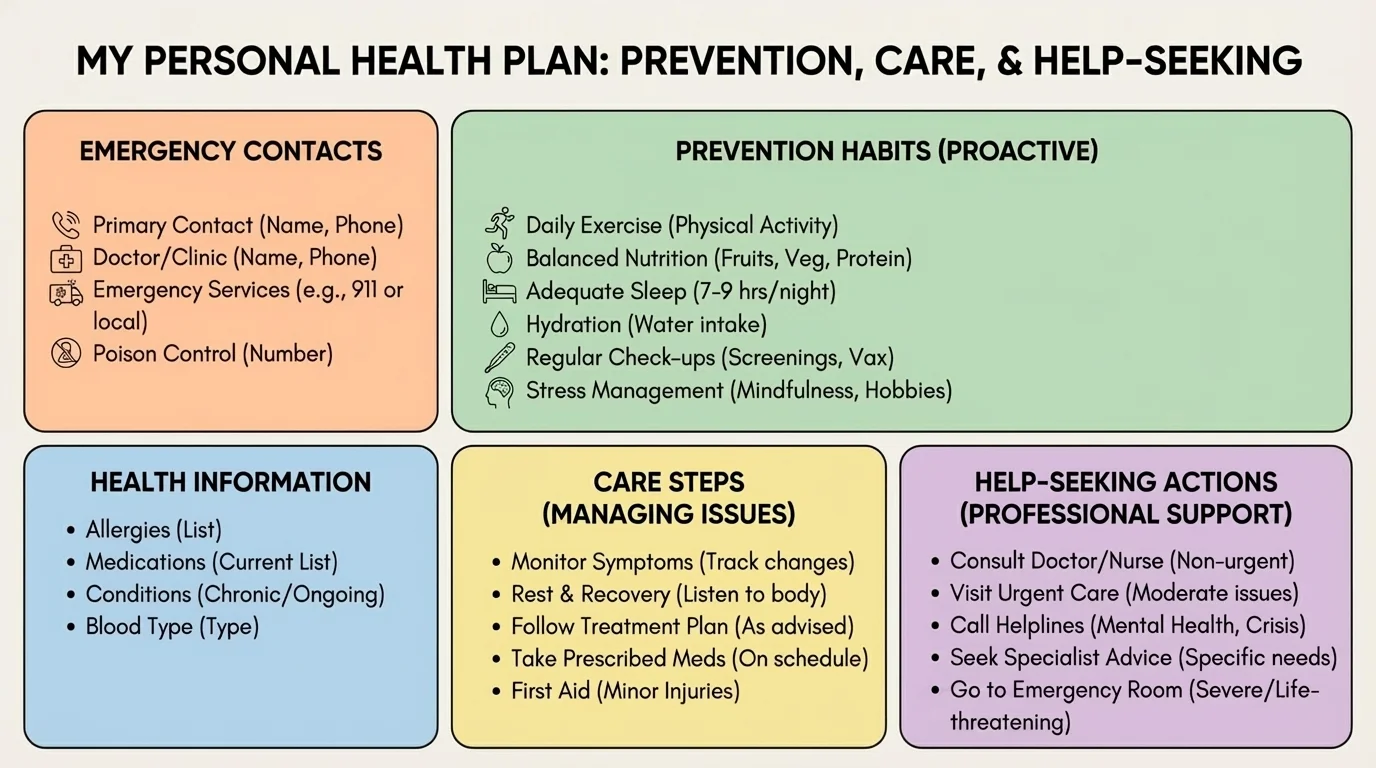
Step 1: Write your key health facts. Include allergies, regular medicines, important diagnoses, and anything first responders or adults should know quickly.
Step 2: List your trusted contacts. Include at least two adults and one healthcare option if possible. Add phone numbers.
Step 3: Write your top prevention habits. Pick realistic ones, not perfect ones. Maybe your list is sleep, water, regular meals, and taking a prescribed medication on time.
Step 4: Add care steps for common issues. Keep them simple: rest, hydrate, tell an adult, check temperature, use approved medication only as directed, monitor symptoms.
Step 5: Add your red-flag symptoms. These are your "do not wait" signs. Trouble breathing, severe allergic reaction, suicidal thoughts with immediate danger, chest pain, fainting, and heavy bleeding are examples.
Step 6: Review and update. If your medicines, contacts, clinic, or needs change, your plan should change too. This is one reason [Figure 3] remains useful later: the same structure still works even when details change.
Try This: Open your phone notes and create five headings right now: "My health info," "Contacts," "Prevention habits," "Home care," and "Get help now if..." Even if you only fill in part of it today, you have started.
Consider Maya, who gets frequent migraines. Her plan includes sleep protection, hydration, known triggers, approved medicine, a dark quiet room, a message template to send her parent, and clear warning signs for when a migraine is unusual and needs medical advice. Because she has a plan, she reacts faster and with less stress.
Now consider Jordan, who notices his mood has been dropping for weeks. He is sleeping badly, losing interest in things he normally enjoys, and feeling overwhelmed. A strong plan tells him not to hide it and hope it disappears. It tells him to contact a trusted adult, describe the pattern clearly, and ask for counseling support. That is prevention and help-seeking working together.
Or think about a sports injury. If your ankle hurts after practice, your plan may say to stop activity, rest, use a cold pack, elevate it, tell an adult, and seek medical evaluation if you cannot bear weight or swelling gets worse. That is much safer than "walking it off" for days.
You do not need to know everything to act responsibly. A good practical plan focuses on your next safe step, not on becoming your own doctor.
The goal is not perfection. The goal is readiness. Life gets busy, symptoms can be confusing, and stress can make thinking harder. Your plan gives you a path when your brain is overloaded.
If your plan is too complicated, you will not use it. Keep it clear, short, and honest. Do not write goals based on who you wish you were on your most organized day. Write a plan based on your real schedule and what you can actually do.
Review your plan every few months, after any major health change, or when you notice it is not working. Maybe your first version says "call the clinic," but you learn that messaging through an app is faster. Maybe your prevention goal was too vague, so you change it. Practical plans improve through use.
Your health plan is also not a replacement for professional care. It is a tool for making good decisions, reducing risk, and speaking up sooner. That makes it one of the most useful life skills you can build now, not later.