Sometimes the most important adult skill is not fixing a problem. It is knowing what to do in the first five minutes when someone says, "I can't do this anymore," stops making sense on a call, sends goodbye messages, or seems completely overwhelmed. In those moments, panic, silence, or guessing can make things worse. Calm, informed action can save a life.
As you move into adulthood, more people may turn to you with serious personal struggles. A friend might text at midnight saying they want to disappear. A coworker might seem severely anxious and unable to function. A sibling might be self-harming, using substances heavily, or talking in a way that sounds detached from reality. You do not need to be a mental health professional to help responsibly, but you do need judgment, boundaries, and a plan.
Mental health crises do not always look dramatic. Some are obvious, like a suicide threat or an overdose. Others are quieter: a friend suddenly withdrawing from everyone, posting messages that sound hopeless, or saying they feel numb and unsafe. Responsible adults learn to notice patterns, take concerns seriously, and connect people with real support instead of hoping the problem will disappear.
Good support can lower danger, reduce isolation, and speed up access to care. Poor support can do the opposite. If you dismiss someone, promise secrecy when you cannot keep it, argue with them, or try to handle a crisis alone, the risk can increase. The goal is not to be perfect. The goal is to be steady, honest, and safe.
"Take every mention of self-harm, suicide, or being unsafe seriously, even if you are not sure how severe it is."
A useful mindset is this: support the person, assess the risk, and connect help quickly. That approach is much more effective than trying to diagnose what is going on.
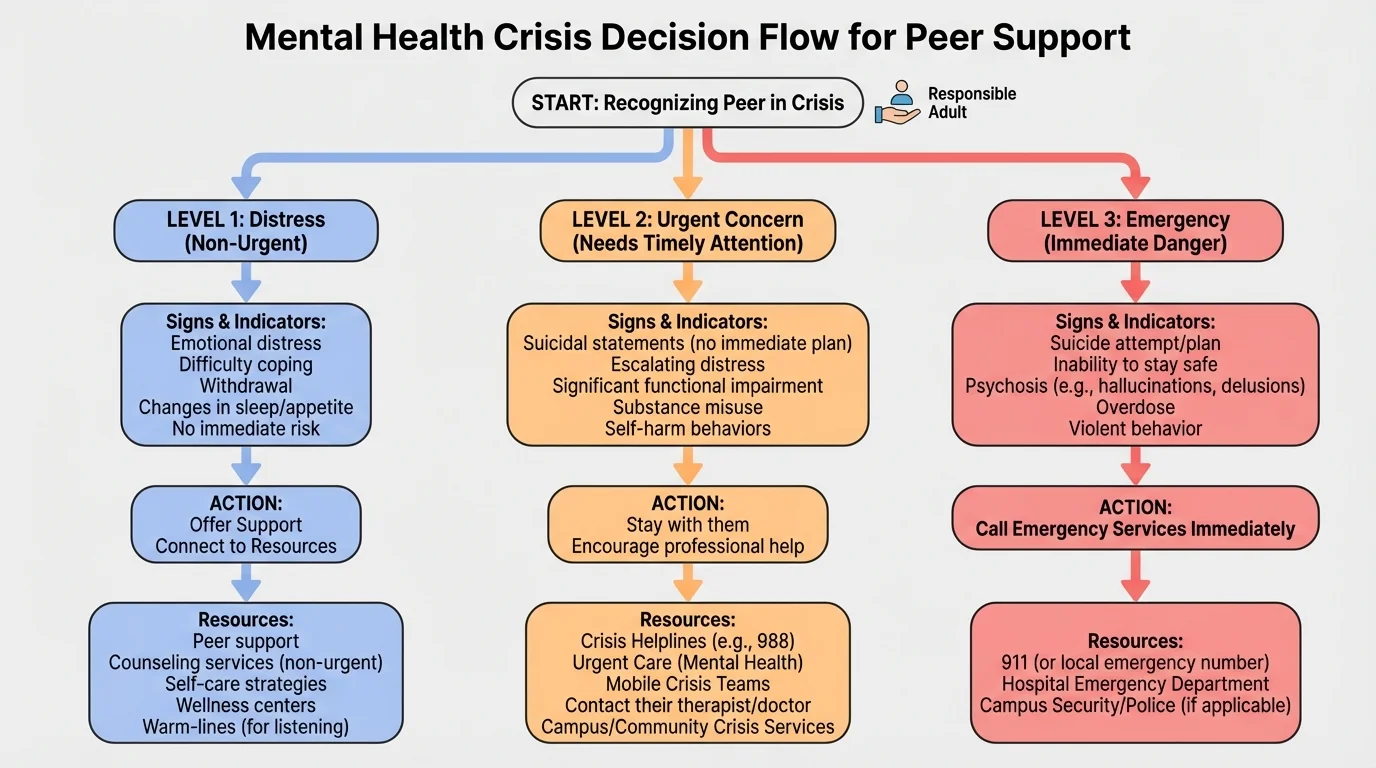
[Figure 1] A mental health crisis is a situation where a person's thoughts, feelings, or behavior create a serious risk to their safety or make it hard for them to function safely. One practical way to sort situations is to think in three levels: distress, urgent concern, and emergency. Distress means the person is struggling but not in immediate danger. Urgent concern means the risk may be rising and outside help is needed soon. Emergency means there is immediate danger and emergency services should be contacted right away.
Warning signs can include talking about wanting to die, saying others would be better off without them, making a plan for suicide, giving away important possessions, severe panic that prevents normal functioning, hearing or seeing things others do not, intense confusion, not recognizing where they are, violent behavior, extreme substance use, or a possible overdose. A person may also stop responding in a coherent way, seem unable to care for basic needs, or say they cannot keep themselves safe.
Suicidal ideation means thoughts about ending one's life. Psychosis involves losing touch with reality, such as hearing voices, seeing things that are not there, or holding beliefs that are clearly disconnected from what is happening. De-escalation means using calm communication and a safe environment to lower emotional intensity and reduce immediate risk.
Not every serious feeling is a crisis, but every possible safety threat deserves attention. If someone says, "I feel depressed," that is important. If someone says, "I have pills next to me and I want this to end," that is an emergency. If someone says, "I keep thinking about hurting myself but I don't know if I will," that is urgent and should not be handled casually.
One mistake people make is waiting for proof. You do not need certainty before you act. If the risk seems possible and the consequences are severe, treat it seriously. That is responsible judgment.
Later, when you decide what kind of resource fits the situation, the urgency levels from [Figure 1] still matter. A person in emotional pain may need a counselor soon; a person who cannot stay safe may need immediate crisis intervention.
Your job is to be a steady bridge to safety, not to become someone's rescuer. That means listening, staying calm, asking direct questions when needed, and involving the right support. It does not mean diagnosing them, promising you will keep dangerous secrets, or making yourself the only person they rely on.
Healthy boundaries matter. If a peer says, "Don't tell anyone," but they also mention suicide, abuse, a weapon, or an inability to stay safe, confidentiality stops there. Safety comes first. Being trustworthy does not mean hiding danger. It means being honest: "I care about you too much to keep this to myself if you might be hurt."
You also need to know your limits. If a friend is having repeated crises and only reaches out to you, that can become unsafe for both of you. Responsible support includes bringing in adults, professionals, hotlines, or crisis teams early instead of carrying the full weight alone.
Support versus rescue
Support means helping someone access safety and care while respecting your limits. Rescue is when you start acting as if their survival depends only on you. Support is sustainable and safe; rescue often leads to burnout, secrecy, and missed warning signs.
In adult life, people respect you more when you respond clearly than when you pretend to have all the answers. A calm "We need more help right now" is often the strongest thing you can say.
Simple sequences help. A practical crisis response process is easier to remember than trying to invent a plan in the moment. Think: notice, assess, ask, stay, connect, and document.
Step 1: Pause and regulate yourself. Take one slow breath. If your mind races, your communication usually gets worse. Speak more slowly than you normally would. Keep your voice and messages simple.
Step 2: Check immediate danger. Ask yourself: Are they talking about suicide, self-harm, harming someone else, a weapon, an overdose, or being unable to stay safe? If yes, move quickly toward emergency or crisis support.
Step 3: Ask direct questions. This is one of the most important adult skills. Asking about suicide does not plant the idea. It can reduce confusion and help you assess danger. You might say, "Are you thinking about killing yourself?" or "Do you feel like you might hurt yourself tonight?" Be respectful, but do not be vague.
Step 4: Stay connected. If the risk is immediate, do not leave the person alone if you can safely stay with them in person, on a call, or by active text contact while help is being contacted. If they are online only, keep them engaged while you gather their location and involve emergency support.
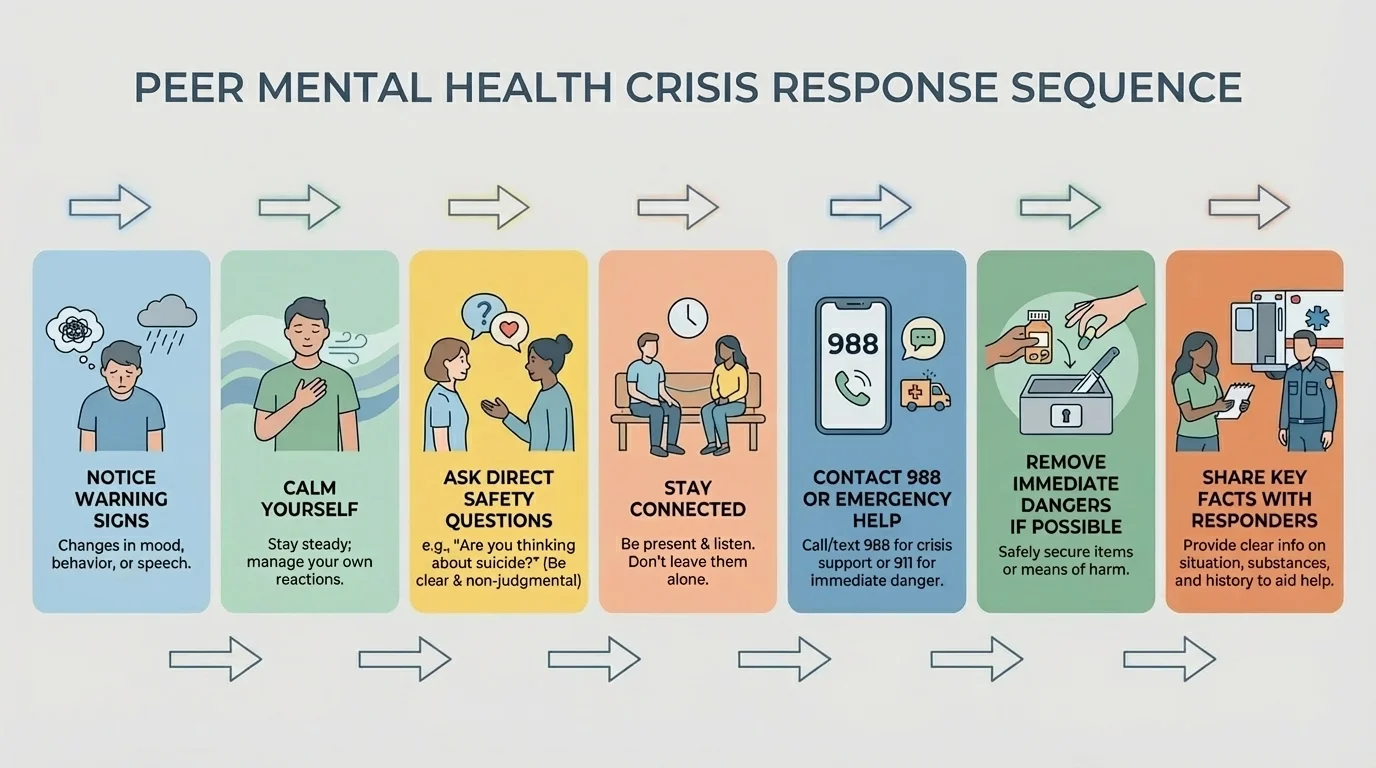
Step 5: Contact the right help. If there is immediate danger, call emergency services. If the person is in the United States and the situation is urgent but not clearly life-threatening, 988 connects you to the 988 Suicide & Crisis Lifeline and local crisis support. Other countries have their own mental health crisis numbers, so it is smart to learn what applies where you live.
Step 6: Share concrete facts. Say what you observed, what the person said, whether there is a plan, whether substances are involved, and where the person is located. Facts help responders act faster. Example: "My friend texted that they took unknown pills about ten minutes ago and said they do not want to wake up. They are at 145 Oak Street, apartment 3."
Step 7: Reduce immediate risk if you can do so safely. That might mean helping move away sharp objects, car keys, pills, alcohol, or firearms. Do not put yourself at risk physically. If the person is aggressive or there is a weapon, emergency services are the priority.
Step 8: Document key details. Save messages, note times, and write down what happened. This is not for drama or gossip. It helps adults, responders, or professionals understand the timeline accurately.
Case study: midnight text from a friend
You receive a message: "I'm done. Don't try to stop me."
Step 1: Respond quickly and directly.
Send: "I'm here. Are you thinking about killing yourself right now?"
Step 2: Keep contact going.
If they reply yes, ask: "What is your address? I'm getting help now. Stay with me."
Step 3: Contact emergency help or 988.
Share the exact messages, their location, and anything you know about means or timing.
Step 4: Notify a responsible adult if possible.
If you know a parent, guardian, older sibling, or roommate who is nearby, contact them immediately.
The most responsible action is not saying the perfect thing. It is getting real help involved fast.
If the person later says, "I was just being dramatic," do not apologize for taking it seriously. It is better to overreact to a possible life-threatening situation than to underreact and be wrong.
The way you speak matters. In a crisis, people often process information poorly. Long speeches, debates, and advice dumps can overwhelm them. Keep your language short, calm, and grounded.
Helpful phrases include: "I'm with you." "You do not have to handle this alone." "I'm concerned about your safety." "Let's get support right now." "Tell me where you are." "Can you move to a safer place while we talk?"
Less helpful phrases include: "Calm down." "Other people have it worse." "You're overreacting." "Promise me you won't do anything." "Just think positive." These statements can feel dismissive or increase shame.
Use active listening. That means reflecting the emotion without pretending to solve everything. For example: "It sounds like you feel trapped and exhausted." "You've been carrying this alone." "I hear that tonight feels especially dangerous." Reflection helps the person feel understood and can lower emotional intensity.
Text-based support has special challenges. You cannot hear tone, and delays can increase fear. If possible, move from text to phone or video. If they refuse, keep messages direct and frequent while you get help. Ask for location early. Screenshots may matter if the situation escalates.
Research and crisis-prevention practice consistently support asking direct questions about suicide when safety is in doubt. Clear questions usually improve assessment and connection rather than increasing risk.
If the person is panicking or becoming overwhelmed, focus on de-escalation by lowering stimulation. Suggest moving to a quieter space, taking slower breaths, sitting down, drinking water, or naming what is around them. If they seem detached from reality or extremely confused, stop trying to reason them out of it and focus on safety and professional help.
Responsible adults know that not all help is the same. Different services fit different levels of urgency. One reason people get stuck is that they hear "get help" but do not know what kind of help actually fits the situation.
[Figure 3] Here are the main categories. A 988 call or text line is for urgent emotional distress, suicidal thoughts, and mental health crisis support. A mobile crisis team may come to the person and assess them on-site. An emergency room is for immediate danger, severe self-harm risk, overdose, violent behavior, or serious medical concerns. An outpatient therapist or counselor is for ongoing support, not for handling an active emergency alone.
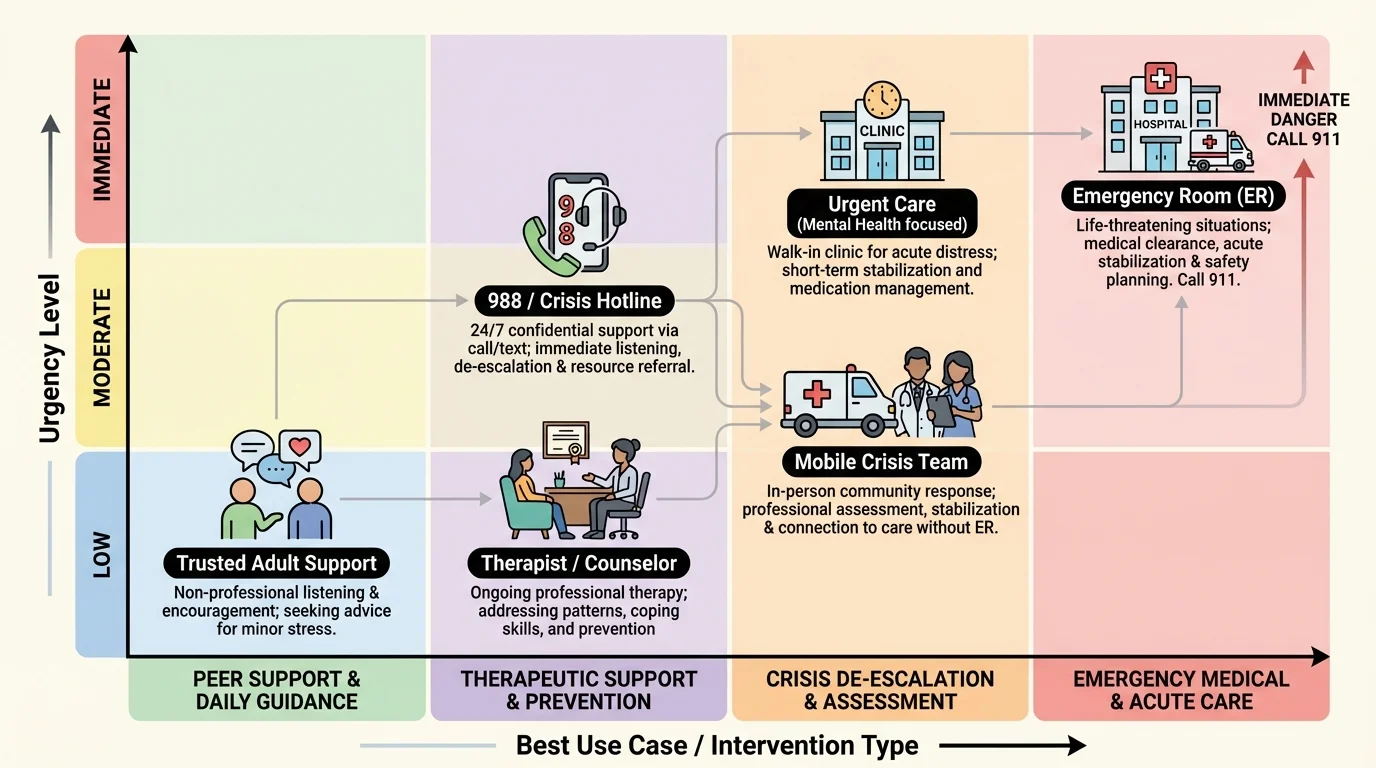
Community resources may also include county mental health agencies, youth and family service organizations, campus counseling centers for older students, support groups, primary care doctors, substance use treatment programs, and domestic violence services. If a peer's crisis includes abuse or coercion, mental health support should be paired with safety planning and victim support resources.
Insurance and cost matter, but they should not delay emergency action. In a crisis, safety comes first. For non-emergency care, help the person look for options such as sliding-scale clinics, community mental health centers, nonprofit counseling programs, telehealth therapy, or assistance through a parent's insurance plan if appropriate.
| Resource | Best for | Not ideal for |
|---|---|---|
| 988 or local crisis line | Suicidal thoughts, urgent emotional crisis, immediate guidance | Long-term weekly therapy |
| Mobile crisis team | Urgent assessment in the community | Situations needing immediate medical stabilization |
| Emergency room | Immediate danger, overdose, severe self-harm risk, medical crisis | Routine emotional support only |
| Therapist or counselor | Ongoing treatment, coping skills, follow-up care | A person who cannot stay safe right now |
| Primary care doctor | Referrals, medication discussions, overall health review | Immediate crisis response alone |
Table 1. Comparison of common mental health resources and the situations they fit best.
The urgency model from [Figure 1] connects directly to resource choice. Distress may call for counseling and follow-up. Urgent concern may call for 988 or same-day assessment. Emergency means emergency services or the emergency room.
"You should talk to someone" is often too vague to help. Effective referrals become concrete actions. When people are overwhelmed, even simple tasks like searching for a phone number, filling out a form, or arranging transportation can feel impossible.
You can help by reducing friction. Offer to sit with them while they call. Help draft a message. Look up clinic hours. Ask whether they want to text 988 together. Help them write down three next steps in their phone notes. If transportation is a barrier, help them identify a safe ride, a nearby adult, public transit, or telehealth options.

A simple referral script sounds like this: "You do not have to figure this out alone. Let's contact 988 now and see what they recommend." Or: "This sounds bigger than what texting can safely handle. I'm going to stay with you while we call your mom and get you to urgent support."
Follow-through matters. If the person agrees to seek help tomorrow, check in tomorrow. Ask, "Were you able to call?" not "Did you feel better?" Concrete follow-up supports action.
Case study: helping a friend connect to therapy after a crisis
Your friend is no longer in immediate danger but is overwhelmed and embarrassed after a crisis call.
Step 1: Normalize the next step.
Say: "A crisis line is a bridge. Ongoing support is what helps you keep going."
Step 2: Make the task smaller.
Help them choose one option: a local clinic, telehealth counselor, or primary care doctor.
Step 3: Reduce barriers.
Offer to help draft the intake email, find insurance information, or plan transportation.
Step 4: Check back with respect.
Send one direct message later: "Just checking whether you were able to make the appointment."
This approach supports responsibility without taking over the person's life.
As this section has shown, practical help often matters more than inspirational words. When stress is high, people need the next step, not a motivational speech.
Some situations require extra caution. If substances are involved, the risk can change fast. Alcohol and drugs lower judgment, increase impulsivity, and can make suicidal behavior more dangerous. If someone may have overdosed, passed out, or mixed substances, treat it as a medical emergency.
If a person seems detached from reality, is speaking in a highly disorganized way, or appears intensely paranoid, safety and professional evaluation matter more than trying to win an argument. You do not need to prove them wrong. You need to keep things calm and get help.
If self-harm is present, do not assume it is "just attention-seeking." Self-harm always signals distress and can escalate. Respond with seriousness and compassion, and involve appropriate support.
Abuse, exploitation, stalking, and threats from others can also trigger crises. In those cases, the plan may need to include law enforcement, domestic violence services, shelter options, or changing passwords and location-sharing settings. Digital safety is part of personal safety.
Cultural respect matters too. Different families and communities talk about mental health differently. Some people fear stigma, immigration concerns, discrimination, or family punishment. Respect those realities, but do not let stigma stop safety action. You can be culturally sensitive and still act quickly.
Supporting someone in crisis can affect you. You might feel guilty, scared, angry, shaky, or exhausted afterward. Those reactions are normal. What matters is what you do next.
After a crisis, debrief with a trusted adult, counselor, supervisor, or another appropriate support person while respecting privacy. You do not need to carry the experience alone. If you feel haunted by what happened, cannot sleep, or keep replaying the conversation, that is a sign you may need support too.
Watch for compassion fatigue, which is emotional exhaustion caused by repeatedly caring for people in distress without enough recovery. Signs include numbness, irritability, dread when your phone buzzes, and feeling responsible for everyone. Caring does not require self-destruction.
Helping well is not the same as helping endlessly. A healthy helper uses support systems, sets limits, and knows when the next right step is to hand the situation to someone more qualified.
Create your own mini safety system now, before you need it. Save crisis numbers in your phone. Know your local emergency number. Identify two adults or mentors you could contact if a peer crisis became too big for you. Learn what mental health resources exist in your community. Preparation makes calm action much more likely.
Being a responsible adult in mental health situations means combining compassion with judgment. You listen, take warning signs seriously, ask direct questions, connect real support, and respect your own limits. That combination protects both the person in crisis and you.